News

On this page we’ll be posting links to articles and information that will help our visitors gain a broader perspective of issues important to us. We will look across the wide spectrum of suicide research, adolescent brain development, and the diagnosis and treatment of depression, anxiety and other mental illnesses. For more links, please see our News Archive page.
February 2024
The Unthinkable Mental Health Crisis That Shook a New England College
Over six terrible months, professors and administrators at Worcester Polytechnic Institute took on the unofficial role of counselors during a spate of campus suicides.
The first death happened before the academic year began. In July 2021, an undergraduate student at Worcester Polytechnic Institute was reported dead. The administration sent a notice out over email, with the familiar, thoroughly vetted phrasing and appended resources…
The week before the academic year began, a second student died. A rising senior in the computer-science department who loved horticulture took his own life. This brought an intimation of disaster. One student suicide is a tragedy; two might be the beginning of a cluster. Some faculty members began to feel a tinge of dread when they stepped onto campus.
The New York Times, Feb. 20, 2024
January 2024
Family of teen who died by suicide warns of dangers of financial sextortion
James Woods, a 17-year-old college-bound track star, had just gotten his driver’s license and posed for his senior yearbook photo when an online predator targeted him on Instagram.
James received 200 messages in less than 20 hours, according to his mother, Tamia Woods.
“It ranged anywhere from ‘I own you,’ to ‘you need to take your own life,'” Woods told CBS News.
The FBI calls what happened to James financial sextortion. “Any child can be a victim of this crime,” said Abbigail Beccaccio, unit chief for the FBI Child Exploitation Unit.
It consists of minors being coerced into sharing compromised images of themselves by criminals who are often working together overseas. The coercion can take place on gaming and video-streaming platforms, or instant messaging apps.
“This is a predator that is solely interested in financial gain,” Beccaccio said.
Children, some as young as 9 years old, are told to send money, or the photos will be posted online.
From October 2021 through March 2023, the FBI tracked roughly 12,600 sextortion victims—all of them minors. Since 2021, at least 20 children who were victims of sextortion have died by suicide, according to the FBI, including James Woods.
CBS Evening News, Jan. 17, 2024
December 2023
Report: 8 Ways to Help Deter Youth Suicide
A new report from The Jed Foundation identifies promising approaches to addressing youth suicide trends for stakeholders in education and beyond.
Suicide is the second leading cause of death for young people ages 12 to 24, with incidents increasing 52 percent between 2000 and 2021, according to data from the Centers for Disease Control and Prevention. U.S. surgeon general Vivek Murthy has put particular emphasis on combating loneliness and suicide among young people, touring colleges around the nation to indicate the need to focus on these issues.
In a new report, published Dec. 6, nonprofit group The Jed Foundation (JED) identifies nine measures institutions and higher education practitioners can take to reduce the number of youth dying by suicide.
Inside Higher Ed, Dec. 20, 2023
Blood Testing Identifies Biomarkers of Suicidal Thoughts: UC San Diego study suggests new way to personalize mental health care
Major depressive disorder affects 16.1 million adults in the United States and costs $210 billion annually. While the primary symptoms of depression are psychological, scientists and doctors have come to understand that depression is a complex disease with physical effects throughout the body. For example, measuring markers of cellular metabolism has become an important approach to studying mental illnesses and developing new ways to diagnose, treat and prevent them.
Researchers at University of California San Diego School of Medicine have now advanced this line of work in a new study, revealing a connection between cellular metabolism and depression. They found that people with depression and suicidal ideation had detectable compounds in their blood that could help identify individuals at higher risk of becoming suicidal. The researchers also found sex-based differences in how depression impacts cell metabolism.
The findings, published December 15, 2023 in Translational Psychiatry, could help personalize mental health care and potentially identify new targets for future drugs.
American Academy of Pediatrics Updates Guidance on Addressing Suicide Risk Among Adolescents
In an updated clinical report addressing adolescent suicide risk, the American Academy of Pediatrics (AAP) offers guidance for pediatricians and pediatric health care providers to assess the possibility of suicide, reduce risks and connect adolescents and their families with mental health resources.
The clinical report, “Suicide and Suicide Risk in Adolescents’” will be published in the January 2024 issue of Pediatrics (online Dec. 11). Clinical reports created by AAP are written by medical experts, reflect the latest evidence in the field, and go through several rounds of peer review before being approved by the AAP Board of Directors and published in Pediatrics.
“Suicide is complex but often preventable,” said Janet Lee, MD, FAAP, one of the authors of the suicide report. “Because of their long-term relationships with teens and their families, pediatricians and other pediatric health care providers are in a unique position to have open communication with young people to discuss mental health and suicidality. This clinical report supports pediatricians in the work they do every day around suicide prevention by helping them recognize risk factors and highlighting evidence-based interventions.”
American Academy of Pediatrics, Dec. 11, 2023
Should schools use AI to detect student suicide risks?
A RAND Corp. report says more evidence is needed to understand the risks and benefits of using online monitoring tools to spot a student crisis.
• Ed tech companies using artificial intelligence-based algorithms to detect risk among students for suicide, self-harm and harm to others via digital monitoring tools can serve as one potentially useful way for schools to prevent suicide, according to a recent RAND Corp. report.
• However, the report found when interviewing parents, advocates and some school staff that concerns persist over the technology’s ability to protect sensitive student data. The study’s respondents also raised flags about the lack of oversight and research regarding the accuracy of AI monitoring tools.
• RAND recommends that school districts engage and get feedback from their communities about the use of AI monitoring tools, inform caregivers and students about any suicide risk surveillance technology in use, and about opt-out policies. Other suggestions for districts include tracking student outcomes following a suicide risk alert and educating students about mental health issues.
Youth suicide rates rose 62% from 2007 to 2021: ‘People feel hopeless,’ one recent grad says
Young people dying by suicide has been an alarmingly frequent headline in recent years.
Katie Meyer, a goalkeeper on the Stanford University women’s soccer team, died by suicide in 2022. She was 22. Ian Alexander Jr., son of actor and director Regina King, killed himself last year. He was 26.
In 2021, an eighth grade boy named Ellis Lariviere took his own life after being told he couldn’t return to the elite private school in Brooklyn, New York, he was currently attending. He was 13.
Last year, suicide rates in the U.S. were the highest they had been since 1941, according to data from the Centers for Disease Control and Prevention.
During the last two decades, youth suicide has increased significantly. From 2007 through 2021, suicide rates for Americans ages 10 to 24 rose 62%, according to the CDC.
November 2023
Suicide rates rose in 2022 overall but declined for teens and young adults
More than 49,000 people died from suicide across the U.S. in 2022, a 3% rise over the year before That’s according to a new report released Wednesday by the U.S. Center for Disease Control and Prevention.
“The number in 2022 is the highest ever recorded in the U.S,” says Sally Curtin, a statistician at the CDC’s National Center for Health Statistics and a lead author of the new report. “These are provisional data, so we expect the final number to actually be a little bit higher than that.”
And the overall suicide rate also went up in 2022 compared to the year before, “the highest that it’s been since 1941,” she adds.
The rate has risen nearly every year since 2000, but there was a brief decline over 2019 and 2020, before the upward trend returned.
‘Kids are struggling’: Suicide rate soaring for Black children and teens nationwide
It’s easy to hear the pride in Gina Smallwood’s voice as she talks about her only son, Kelvin.
“His first little job was at the elementary school library,” she said. “He was just really, really bright, very talented, athletic.” A talented boy who became an honor roll student at Morehouse College in Atlanta.
“So many other adults will be like, ‘we love Kelvin’ and I will be like, I love him, too,” she said. Weeks before Kelvin’s 20th birthday, Smallwood said she got a call she would never forget. “That’s when the officer said, ‘Ms. Smallwood, we found your son and he’s dead,” she said.
This was February 2008. Smallwood said she was traveling from Atlanta to Washington D.C. when Kelvin took his own life. She said he used her own gun that had been locked up in her bedroom.
His memorial was March 8, the day that would have been his 20th birthday. “That was a really, really like numb time and I walked around numb for probably almost two years,” said Smallwood.
Understanding and addressing Teen Suicide: A call for support and prevention
Teen suicide is a deeply concerning issue that continues to affect individuals, families, and communities worldwide. The loss of young lives to suicide is a tragedy that leaves a lasting impact on society. It is crucial to understand the underlying factors contributing to this alarming trend and explore effective strategies for prevention and support. By shedding light on the complexities of teen suicide, we can work together to create a safer and more nurturing environment for our young people.
Teen suicide is a multifaceted issue with myriad causes and contributing factors. Some of the common elements include: Mental Health Challenges: Mental health disorders such as depression, anxiety, bipolar disorder, and substance abuse significantly increase the risk of suicide among teens. Untreated or undiagnosed mental health conditions can exacerbate feelings of hopelessness and despair.
People’s Defender, Nov. 23, 2023
This Is Not the Way to Help Depressed Teenagers
Ever since the pandemic, when rates of teenage suicide, anxiety and depression spiked, policymakers around the world have pushed to make mental-health resources more broadly available to young people through programming in schools and on social media platforms.
This strategy is well intentioned. Traditional therapy can be expensive and time-consuming; access can be limited. By contrast, large-scale, “light touch” interventions—TikTok offerings from Harvard’s School of Public Health, grief-coping workshops in junior high—aim to reach young people where they are and at relatively low cost.
But there is now reason to think that this approach is risky. Recent studies have found that several of these programs not only failed to help young people; they also made their mental-health problems worse. Understanding why these efforts backfired can shed light on how society can—and can’t—help teenagers who are suffering from depression and anxiety.
The New York Times, Nov. 18, 2023
October 2023
David Shaffer, Medical ‘Detective’ in Suicide of Youths, Dies at 87
At a time when teen suicide was seen as random and unpredictable, Dr. Shaffer, a psychiatrist, led investigations that proved that it was not.
Dr. David Shaffer, a psychiatrist who spent decades studying children and teenagers who died by suicide, constructing a framework for screening and laying the groundwork for modern prevention efforts, died on Sunday in Mastic Beach, N.Y., on Long Island. He was 87.
His son, Dr. Charlie Shaffer, said the cause was respiratory complications of Alzheimer’s disease. For about six years, as the disease progressed, he had lived on the estate of the Vogue editor Anna Wintour, his former wife and the mother of two of his children.
In the 1970s, when Dr. Shaffer was a young doctor, most people saw the suicide of a child or adolescent as a random and unpredictable act. Trained as an epidemiologist, he undertook an investigation known as a “psychological autopsy,” gathering detailed information from adult caregivers of 31 children who had died by suicide.
The research yielded surprises. In more than a third of the cases, the suicide had occurred in the midst of what he called a “disciplinary crisis,” as the child awaited consequences. Many of the children were described, not as depressed, but as aggressive or impulsive.
The New York Times, Oct. 18, 2023
Skyrocketing teen boy suicides linked to firearms access: Mental health experts say stigma about masculinity can lead to deadly outcomes
Suicide rates were 3.2 times higher for teenage boys than teen girls between 2018 and 2020 — with guns increasingly playing an outsize role. Boys and young men represent 80% of all youth suicide deaths, with 90% of all those who die by suicide using a firearm.
“Few people know that the majority of gun deaths in this country are actually suicides,” said Nina Vinik, founder and executive director of Project Unloaded, an organization that works with teens and adolescents to make data-backed decisions to reduce the risk of being hurt by gun violence. “When most people think about gun violence, they tend to think about interpersonal gun violence, which is certainly important — but really overlooks the crisis that we are facing with firearm suicide.”
Suicide is the second leading cause of death among people ages 15 to 24 in the United States, and suicide rates for 15- to 19-year olds have jumped by 29% in the past 10 years.
Vinik noted that the suicide rate, already at a 20-year high, is rising the most quickly among young people of color. And in terms of how youths are dying, young men of color are seeing firearm suicide rates increase “exponentially, by triple digits. This is having a particularly devastating impact on young people of color and I think this has really been overlooked in the data.”
How To Talk About Suicide With Children?
Informing kids about suicide is difficult, but addressing their fears is vital.
Parenting makes it hard to express such a painful circumstance. Consider adapting terminology to your child’s age and cognitive ability, and be direct and honest with them. This article offers tips for discussing suicide with kids responsibly and conveniently.
A 2021 study by the International Association for Suicide Prevention predicts an estimated 703,000 annual suicides. Communication is a key preventative strategy, especially when opening the conversation with kids.
This issue seldom occurs until a specific circumstance prompts parents to discuss suicide with their children. This conversation is impending when a close relative commits suicide or attempts to, a child has heard the term but doesn’t know what it means, or the parents approach the child to discuss a topic connected to their current situation.
September 2023
Suicide rates of teenage boys are skyrocketing because of firearm access
Experts on adolescent suicide say too often, guns and stigma around masculinity and mental health lead to deadly outcomes.
September is National Suicide Prevention Month and The 19th is looking at how gender factors into the political and cultural forces at play in suicide prevention.
Suicide rates were 3.2 times higher for teenage boys than teen girls between 2018 and 2020 — with guns increasingly playing an outsize role. Boys and young men represent 80 percent of all youth suicide deaths, and 90 percent of all those who die by suicide using a firearm.
“Few people know that the majority of gun deaths in this country are actually suicides,” said Nina Vinik, the founder and executive director of Project Unloaded, an organization that works with teens and adolescents to make data-backed decisions to reduce the risk of being hurt by gun violence.
“When most people think about gun violence, they tend to think about interpersonal gun violence, which is certainly important — but really overlooks the crisis that we are facing with firearm suicide.”
Suicide is the second leading cause of death among people ages 15 to 24 in the United States, and suicide rates for 15- to 19-year olds have jumped by 29 percent in the past 10 years.
Teens May Consider Suicide More Than Parents Realize: Doctor Shares How to Help
Many parents would agree that they know their child well. They believe they can easily read their child’s expressions and emotions and would immediately know if something was seriously bothering them. However, it’s important to recognize that even in close relationships, there can still be moments when a child conceals their emotions or internal struggles.
In fact, many parents often have no idea that their children may be considering or thinking about suicide. According to a study published by the American Academy of Pediatrics, half of parents don’t know their child has had thoughts about suicide, and three in four parents are unaware of their child’s thoughts of death and dying.
There can be several reasons for this disconnect, including lack of communication, the stigma around mental health issues, developmental factors, and online and peer influence, to name a few.
Iredell Health System, Sept. 25. 2023
As younger children increasingly die by suicide, better tracking and prevention is sought
Jason Lance thought Jan. 21, 2010, was a day like any other until the call came.
He had dropped off his 9-year-old son, Montana, at Stewart’s Creek Elementary School in The Colony, Texas, that morning.
“There were no problems at home. He was smart. He wore his heart on his sleeve and he talked and talked and talked,” said Lance. It was “the same old, same old normal day. There were kisses and goodbyes and he said, ‘I love you, Daddy.'”
A few hours later, school officials called to say Montana had died by suicide while locked in the nurse’s bathroom.
“I knew he had some issues going on in school, but I never seen it coming,” said Lance. His shock and grief were complicated by the realization that there may have been more signs his son was struggling.
Students Struggling With Suicide
Q&A Children and young adults may have a difficult time during the back-to-school season, particularly if they experience suicidal thoughts or suicidal ideation. Psychiatric Times sat down with Jill Harkavy-Friedman, PhD, senior vice president of research at the American Foundation for Suicide Prevention, to examine the complex topic of suicide in young students.
PT: What issues might arise for students struggling with suicidal ideation as they head back to school?
Harkavy-Friedman: Returning to school can be a source of mixed emotions for any student. It is a complex time for students who have been struggling with suicidal ideation during the summer. Returning to school can increase stress, exacerbate concerns about feeling stigmatized or not belonging, and lead to difficulty connecting with their peers. In order to support students, help them take care of basics such as sleep, diet, exercise, and hydration. It is a good time to have open, nonjudgmental conversations about their thoughts and feelings and practice ways to manage discomfort.
Psychiatric Times, Sept. 6, 2023
AI identifies top predictors of adolescent suicide and self-harm
Researchers have used a machine learning algorithm to identify the top factors that can predict an adolescent’s risk of self-harm and attempting suicide. They say their model is more accurate than existing risk predictors and could be used to provide individualized care to vulnerable patients.
Adolescence is a critical formative period. Physical, emotional, and social changes can make adolescents vulnerable to mental health problems, including suicide attempts and self-harm. According to the Australian Institute of Health and Welfare (AIHW), suicide is the leading cause of death amongst Australians aged 15 to 24. In the US, the Centers for Disease Control and Prevention (CDC) lists it as the second leading cause for 10-to-14-year-olds.
The standard approach for predicting suicide or self-harm relies on past suicide or self-harm attempts as the only risk factor, which can be unreliable. Now, researchers led by the University of New South Wales Sydney have used machine learning (ML) to accurately identify the top factors that place adolescents at increased risk of suicide and self-harm.
August 2023
Why are American teenagers feeling hopeless? The youth mental health crisis, explained
According to a new poll from the Centers for Disease Control and Prevention, teenagers in America are experiencing an unprecedented mental health crisis. 29 percent of boys and 57 percent of girls reported “persistent feelings of sadness or hopelessness” and levels of reported sexual violence were up significantly from pre-pandemic baselines.
Those numbers were even higher for LGBTQ+ students, including 45 percent of girls in that category reporting seriously considering suicide at some point in 2021. What is driving this worrying deterioration in youth mental health, and what are experts suggesting can be done about it? Here’s everything you need to know about America’s youth mental crisis.
The CDC’s data was collected in fall 2021, as part of the agency’s Youth Risk Behavior Surveillance System (YRBS), which has been conducting survey research since 1991. The patterns it identifies are concerning on a number of fronts beyond the toplines in media reports. Rates of attempted suicide, for example, climbed to their highest levels in more than a decade.
A shocking 13 percent of high school girls and 7 percent of high school boys reported a suicide attempt in 2021. Meanwhile, 24 percent of girls reported “making a suicide plan,” a 9-point increase from 2011, along with 12 percent of boys (up one point). The percentage of high school girls who contemplated suicide (30 percent) was almost double what it was in 2011. Almost one in four LGBTQ+ students were bullied or experienced sexual violence at school, and as a consequence, many chose to stay home.
The Week, Feb. 26, 2023 (posted 08/14/23)
U.S. Suicide Deaths Rose in 2022, C.D.C. Estimates Say
Provisional data from the Centers for Disease Control and Prevention show that deaths by suicide were up last year — but not for all groups.
The estimated number of suicide deaths in the United States rose to nearly 50,000 in 2022, according to provisional data released on Thursday from the Centers for Disease Control and Prevention. The total would be an increase of approximately 2.6 percent since 2021.
The C.D.C. estimates the overall number of deaths to be 49,449 but has not yet calculated the suicide rates for 2022. Given that the U.S. population grew by about 0.4 percent in 2022, a 2.6 percent increase in deaths indicates that suicide rates are continuing to rise, although not universally among all groups.
Suicide deaths have fluctuated somewhat over the years and declined in 2019 and 2020. But the overall suicide rate, or the number of suicides per 100,000 people, has increased by about 35 percent over the last two decades. People 65 and older had the highest increase in the number of deaths by suicide in 2022 among the various age groups.
The New York Times, August 11, 2023
Suicide Down 8.4 Percent Among Teens and Young Adults
Suicides decreased by 8.4 percent among 10-to-24-year-olds last year, according to provisional data released by the Centers for Disease Control and Prevention (CDC).
The drop in teen and young adult suicides is a bright spot among an overall bleak portrait of U.S. suicide rates in 2022.
Overall, 49,449 Americans are known to have killed themselves last year—the highest number of U.S. suicides on record and an increase of 2.6 percent over 2021. The CDC “has not yet calculated a suicide rate for the year, but available data suggests suicides are more common in the U.S. than at any time since the dawn of World War II,” reports the Associated Press.
The biggest increases occurred in older and middle-age adults. Suicides were up by 8.1 percent among Americans ages 65 and above. And they increased by 6.6 percent among adults ages 45 through 64. Among adults ages 25 through 44, suicides were up by 0.7 percent.
Disordered Sleep Linked to Increased Risk of Suicide in Youth
Emergency department records reveal that youth experiencing disrupted sleep are at greater risk for suicidal thoughts and behaviors.
Youth who experience disrupted or disordered sleep were found to be at increased risk for suicidal thoughts and behaviors, in a recent analysis of emergency department (ED) records.1
“Being aware of the impact of sleep disruption gives us an avenue to try to address sleep issues as well as downstream consequences,” explained study co-author, Melynda Casement, PhD, Department of Psychology, University of Oregon, in an announcement of the study publication.
“Suicide is still stigmatized in many communities; sleep is less so,” she observed. “Identifying and treating sleep disorders could improve mental health and reduce suicide risk even if [individuals] are not comfortable opening up about their mental health challenges.”
Psychiatric Times, Aug. 7, 2023
July 2023
Teen Suicide Plummeted During Covid-19 School Closures, New Study Finds
Rates of suicide and suicide attempts among teenagers were at their lowest when schools were closed for the Covid-19 pandemic, a new study published Wednesday shows, pointing to an overall pattern that shows mental health in children and teenagers is at its worst while school is in session.
Researchers with the University of Texas’s Houston School of Public Health studied more than 73,000 emergency department visits and hospitalizations between 2016 and 2021, of which there were an average of 964 suicide-related visits per 100,000 children between ages 10 and 18 each year.
The rate of suicidality among young people, which has been increasing for a decade, rose from 760 per 100,000 children in 2016 to 1,006 in 2019 before an unexpected decrease in 2020—the first year of the pandemic—brought the rate down to 942.
The study also found peaks in suicidal ideation in April and October of most years, with a dramatic low in the summer months when school was not in session, but in 2020 saw a disruption in that seasonal pattern with the lowest suicidality rates in April and May—when schools were closed for Covid.
Teens have increasingly wound up in the hospital for suicidal thoughts and attempts, study shows
The research found a seasonal pattern in emergency room visits and hospitalizations related to suicide attempts and ideation among young people.
Hospitalizations and emergency room visits for suicide attempts and ideation rose nationally among children and teens from 2016 to 2021, a new study has found — the latest in a series of alarm bells about the state of young people’s mental health.
According to the research, published Wednesday in the journal JAMA Network Open, nearly 66% of the cases were girls, and the average age was 15. The study also revealed seasonal trends: ER visits and hospitalizations were 15% higher in April and 24% higher in October than the January rate, which the study used as a baseline because it was close to the annual average. However, 2020 was an exception both to the seasonal fluctuations and the increase in suicidality over time.
Taken as a whole, the researchers said the findings indicate that the academic calendar may affect youth mental health.
Online, ‘unalive’ means death or suicide. Experts say it might help kids discuss those things
Language has always evolved, and new words have always popped up. In this case, words were created within a digital setting to evade rules and are permeating spoken language, especially among youths.
This story includes discussion of suicide. If you or someone you know needs help, please call the National Suicide Prevention Lifeline at 988 or 1-800-273-8255.
When Emily Litman was in middle school, kids whose parents grounded them would blithely lament: “I just want to die.” Now she’s a middle school teacher in New Jersey, and when her students’ phones and TikTok access are taken away, their out-loud whining has a 21st-century digital twist: “I feel so unalive.”
Litman, 46, teaches English as a second language to students in Jersey City. Her students don’t use — and perhaps have never even heard — English words like “suicide.” But they know “unalive.”
“These are kids who’ve had to learn English and are now learning TikToklish,” Litman says.
“Unalive” refers to death by suicide or homicide. It can function as adjective or verb and joins similar phrasing — like “mascara,” to mean sexual assault — coined by social media users as a workaround to fool algorithms on sites and apps that censor posts containing discussion of explicit or violent content.
Language has always evolved. New words have always popped up. Teenagers have often led the way. But the internet and online life pave the way for it to happen more quickly.
WUSF Public Media, July 15, 2023
An Elite School, a Boy’s Suicide and a Question of Blame
An eighth grader was asked to leave Saint Ann’s, a prestigious private school in Brooklyn. Three months later, he ended his life. Now his parents are suing the school.On Feb. 3, 2021, the school informed his mother by email that, “despite recent progress,” he could not return for ninth grade.
Ellis asked his parents if it was the school’s decision or theirs. When they told him, “he just cried a lot,” his mother, Janine Lariviere, said. “He didn’t want comfort from me. He was very hurt. This is the most painful thing for me, because I didn’t know how to protect him.”
Three months later, in the family home in Red Hook, Brooklyn, Ellis ended his life. He was 13.
This April, his parents filed suit against the school, its head and its trustees, arguing that its practices caused their son’s death and demanding changes in school policies. In their suit, they quote the last line of Ellis’s suicide note: “Don’t let the school do an assembly about this.”
The New York Times, July 2, 2023
June 2023
Suicides, homicides surged early in pandemic for youths
The homicide rate for older U.S. teenagers rose to its highest point in nearly 25 years during the COVID-19 pandemic, and the suicide rate for adults in their early 20s was the worst in more than 50 years, government researchers said Thursday.
The Centers for Disease Control and Prevention report examined the homicide and suicide rates among 10- to 24-year-olds from 2001 to 2021.
The increase is alarming and “reflects a mental health crisis among young people and a need for a number of policy changes,” said Dr. Steven Woolf, a Virginia Commonwealth University researcher who studies U.S. death trends and wasn’t involved in the CDC report.
Experts cited several possible reasons for the increases, including higher rates of depression, limited availability of mental health services and the number of guns in U.S. homes.
Guns were used in 54% of suicides and 93% of homicides among the age group in 2021, the most recent year for which statistics were available.
The Times Leader, June 26, 2023
Suicide rate increased 60% since 2011 among US youth and young adults: CDC report
The rate rose from 6.9 per 100,000 in 2001 to 11 per 100,000 in 2021.
Deaths from suicide among youth and young adults have been increasing over the last two decades in the United States, new federal data showed.
For those between the ages of 10 and 24, the suicide rate remained stable between 2001 and 2007, around 6.9 per 100,000.
From 2011, the rate rose 60% to 11.0 per 100,000 in 2021, according to a report published early Thursday by the Centers for Disease Control and Prevention’s National Center for Health Statistics.
“You don’t want to see rates of suicide go up and so, in that sense, it isn’t surprising, unfortunately, because the trendline has been going up,” Dr. Madhukar Trivedi, a professor of psychiatry at UT Southwestern Medical Center, told ABC News.
5 Ways Teens Can Protect Their Mental Health on Social Media–New guidance teaches teens how to use social media in healthier ways.
• Social media’s role in the current national youth mental health crisis raises concern for the Surgeon General.
• The advisory on social media and youth mental health recommends that teens develop healthy screen practices.
• Teens must gain skills for informed decision-making, seeking support, and prioritizing mental health.
With up to 95 percent of all youth between 13 and 17 years old being social media users, it is evident that social media is an integral part of the Gen Z way of life. Additionally, despite the minimum age requirement being 13 on most social media platforms, a whopping 40 percent of children aged 8 to 12 are social media users.
“We are in the middle of a national youth mental health crisis, and I am concerned that social media is an important driver of that crisis — one that we must urgently address,” said U.S. Surgeon General Vivek Murthy in a recent interview.
Psychology Today, June 10, 2023
May 2023
Suicide is the new epidemic plaguing Black youth
As Mental Health Awareness Month draws to a close, it is necessary to discuss a dangerous issue in the Black community. No mincing of words here. There is a new epidemic plaguing our youth. According to the Association of American Medical Colleges, Black young people aged 10-19 experienced a 78 percent increase in suicide in comparison to other races. When you delve into the other age subgroups, the results are even more sobering.
A research study conducted by the AAMC found that younger children, aged 5-12, were twice as likely to commit suicide than white children in the same age demographic. What is causing our youth to have such a bleak outlook on life that they are willing to take their own after brief stints here on Earth?
COVID-19’s Ripple Effect: The Youth Suicide Surge
A recent study found that suicide rates among US youth aged 5-24 years increased during the COVID-19 pandemic, particularly among males, preteens, young adults, and specific racial and ethnic groups. This highlights disparities that have likely been worsened by the pandemic and underscores the need for targeted suicide prevention efforts.
Suicide is a leading cause of death among young people in the United States. Rates of youth suicide deaths were rising before the coronavirus (COVID-19) pandemic began, so it is critical to understand how the pandemic impacted this public health crisis. In a new study supported by the National Institute of Mental Health, researchers examined national youth suicide trends and characteristics in the United States before and during the COVID-19 pandemic.
Does Social Media Harm Young People’s Mental Health?
The United States surgeon general issued an extraordinary public warning that could bring changes to how young people use the platforms. What is your reaction?
On Tuesday, Dr. Vivek Murthy, the United States surgeon general, issued a rare public health advisory on the risks that social media may pose to young people’s mental health and well-being. The report explains:
A Surgeon General’s Advisory is a public statement that calls the American people’s attention to an urgent public health issue and provides recommendations for how it should be addressed. Advisories are reserved for significant public health challenges that require the nation’s immediate awareness and action.
The New York Times, May 25, 2023
New report reveals drastic increase in youth suicide.
Teens are struggling with more mental health challenges nationwide.
In 2021, 1767 teens died by suicide in the US and all of them under the age of 17.
This is one of the findings from a new national report about youth well-being released by Trust for America’s Health, a public health organization, on Wednesday.
It shows the youth suicide rate for teens increased by 71 percent between 2010 and 2021.
“Calling attention to what has been a long-standing mental health crisis,” said Dr. Nadine Gracia, President and CEO of Trust for America’s Health.
Dr. Gracia said LGBTQ youth are even more at risk.
“Not feeling that they’re having the support and approval and that’s in different settings like at home with their family or in their school if they feel they’re being bullied,” she said.
This same report also outlines recent federal data from the CDC about these trends.
It shows LGBTQ high school students were nearly four times as likely to attempt suicide compared to heterosexual teens in 2021.
How Do You Actually Help a Suicidal Teen?
It’s a dark time for therapists treating adolescents in despair. But some things do work.
Suicidal children are caught in a vortex of pain, and those around them are often unsure how to respond. Some pediatricians, as well as therapists, school counselors and others, lack the training to best help a teenager who reveals suicidal thoughts, leaving parents to wonder what to do. At what point do you take your child to the hospital? What if they refuse to go? If they have attempted suicide, do you consider residential care in a facility, where children live for weeks or months at a time? What else can you do to protect them? How do you know they won’t die the next time? You lock up your medications, your kitchen knives, your guns if you have them. You find a good therapist, if you’re lucky. But a teenager can always find a way. What alarm system, safety locks or rules guard against a desperate child’s resourcefulness?
The New York Times, May 17, 2023
Suicide rates for girls are rising. Are smartphones to blame?
Hospitalisation rates for self-harm have increased by 140% since 2010.
In 2017 jean twenge, a professor at San Diego State, wrote an essay entitled “Have smartphones destroyed a generation?” Her answer, “yes”, was provocative at the time. Now, it is a common refrain. Spurred by recent data showing a rise in depression among American teenagers, both the British and American press have barraged readers with stories about social media ravaging young people’s mental health. Jonathan Haidt of New York University has compared social media to waterboarding. The public has noticed: in a recent survey, 53% of Americans said that social media were mostly or fully responsible for increasing teenagers’ depression.
Smartphones went global long ago. If they are causing an epidemic of sadness, evidence should appear around the world. Data support the claim that young people, particularly girls, have deteriorating mental health. But they leave room for doubt that mobiles are the main culprit.
Almost a Third of High-School Girls Considered Suicide in 2021
Nearly a third of female high-school students said they had considered suicide in 2021, a significant increase since 2019 and a strong signal that teenagers need better and broader mental-health support, according to recent data from the U.S. Centers for Disease Control and Prevention (CDC).
For years, researchers have tracked a concerning dip in the mental health of America’s teen girls. In 2021, nearly 60% of U.S. teenage girls said they felt sad or hopeless—the highest number in a decade, and roughly double the one reported among teenage boys that year. But the problem predates the pandemic. Depression has become more common among young people over the past decade, and in 2015, after years of increases, the suicide rate among teenage girls hit a 40-year high.
Suicide Rates Among U.S. Adolescents Doubled in 10 Years
Suicides among the youngest U.S. teenagers were rising for years before the pandemic — with school stress, social media and guns standing as potential factors, according to a new study.
Researchers found that between 2008 and 2018, the suicide rate among 13- and 14-year-olds nationwide more than doubled — from roughly two deaths per 100,000 teens in 2008, to five per 100,000 a decade later.
It was a stark reversal of a decline that began in the late-1990s.
U.S. News & World Report, May 1, 2023
After Student’s Suicide, an Elite School Says It Fell ‘Tragically Short’
The Lawrenceville School in New Jersey on Sunday made a remarkable admission of failure and committed to a new focus on mental health.
Last April, Jack Reid, a 17-year-old junior at one of the nation’s elite boarding schools, tucked a Bible into his gym shorts and a note into his pocket directing his parents to a Google document explaining his feelings of despair. Then, inside his dorm room, he took his own life.
On Sunday, the anniversary of Jack’s death, the Lawrenceville School in New Jersey offered an extraordinary admission of failure, publicly acknowledging that it had been aware that Jack was being bullied by other students, but that it had fallen “tragically short” of its obligation to protect him.
“The school acknowledges that bullying and unkind behavior, and actions taken or not taken by the school, likely contributed to Jack’s death,” Lawrenceville officials wrote in a statement posted Sunday morning on the school’s website.
The New York Times, May 1, 2023
April 2023
One-third of US teen girls seriously considered attempting suicide in 2021: CDC
The number of teen girls who made a suicide plan also increased from 2019.
The number of teenage girls experiencing suicidal thoughts and behaviors increased during the second year of the pandemic, new federal data showed.
The percentage of high school female students who seriously considered attempting suicide rose from 24.1% to about one-third, or 30%, between 2019 and 2021, according to the latest results of the Youth Risk Behavior Survey, published Thursday by the Centers for Disease Control and Prevention.
The percentage of those who made a suicide plan increased from 19.9% to 23.6% and there was also an increase in suicide attempts from 11.0% to 13.3%, according to the CDC survey.
Differences were seen when it came to students’ ages, race/ethnicity or gender identity.
Alarming Rates of Teen Suicide Continue to Increase in the U.S.
In the United States suicide has become the second leading cause of premature death among those ages 10 to 24; it is the leading cause of death among teens ages 13 to 14.
Researchers from Florida Atlantic University’s Schmidt College of Medicine and collaborators conducted a study exploring trends in rates of suicide among 13 to 14 year olds in the U.S. from 1999 to 2018. They also explored possible modifications by sex, race, level of urbanization, census region, month of the year and day of the week.
Results, published online ahead of print in the journal Annals of Pediatrics and Child Health, showed that among children ages 13 to 14, suicide rates more than doubled from 2008 to 2018, following a rise in social media and despite significant declines in suicide mortality in this age group previously from 1999 to 2007. These trends were similar in urban and rural areas but were more common in boys in rural areas where firearms are more prevalent.
These statistically significant increasing trends were similar by sex, race, urbanization and census regions. In rural areas, firearms were used in 46.7 percent of suicides in boys and 34.7 percent in metropolitan areas. Suicides occurred significantly more often between September and May and were highest on Monday followed by the rest of the weekdays, suggesting school stress as a contributor.
Florida Atlantic University, April 26, 2023
Attempted suicide by poisoning among children rises 30% in two-year span, UVA study finds
The rate of suspected suicide attempts by poisoning among children and adolescents ages 10-19 reported to U.S. poison centers increased 30% during 2021 – the COVID-19 pandemic’s first full year – compared with 2019, a new UVA Health study found.
The study found the rate of suspected suicide attempts by poisoning among children ages 10-12 increased 73% during 2021 compared with 2019. Among adolescents ages 13-15, the rate of suspected suicide attempts by poisoning increased 48.8% in 2021 versus 2019. The rate of suspected suicide attempts by poisoning among females ages 10-19 increased 36.8% in 2021 compared with 2019.
The findings are based on a review of cases reported to the National Poison Data System by U.S. poison centers as “intentional suspected suicide,” which encompass both suspected suicide attempts and intentional self-harm, according to a UVA news release.
Girls accounted for 81.2% of the suspected suicide attempts among adolescents ages 10-19 in 2021, compared with 77% in 2019.
The increases in suspected suicides occurred while overall calls to the nation’s poison centers decreased 3.1% from 2019 to 2021.
Suspected Suicide Attempts by Self-Poisoning Among Persons Aged 10–19 Years During the COVID-19 Pandemic — United States, 2020–2022
What is already known about this topic?
In 2020, suicide was the second leading cause of death among persons aged 10–14 years and the third leading cause among those aged 15–24 years.
What is added by this report?
Analysis of National Poison Data System data found that the rate of suspected suicide attempts by self-poisoning among persons aged 10–19 years increased 30.0% in 2021 as compared with prepandemic rates (2019), with a 73.0% increase among children aged 10–12 years, 48.8% among adolescents aged 13–15 years, and 36.8% among females.
What are the implications for public health practice?
A comprehensive public health approach to suicide prevention measures focusing on children and adolescents and involving partnerships among families, school teachers, mental health professionals, and public health leadership is needed.
TikTok’s Algorithm Keeps Pushing Suicide to Vulnerable Kids
The superpopular app can serve up a stream of anxiety and despair to teens. TikTok says it’s making improvements but now faces a flood of lawsuits after multiple deaths.
TikTok’s algorithm doesn’t know Chase Nasca is dead.
More than a year after Nasca killed himself at age 16, his account remains active. Scroll through his For You feed, and you see an endless stream of clips about unrequited love, hopelessness, pain and what many posts glorify as the ultimate escape: suicide.
“Take the pain away. Death is a gift,” says one video pushed to the account this February, days before the first anniversary of Nasca’s death. In another, a male voice says, “I’m going to put a shotgun in my mouth and blow the brains out the back of my head,” and a female voice responds: “Cool.”
The feed looked much the same in the days before Nasca died. On Feb. 13, 2022, it surfaced a video of an oncoming train with the caption “went for a quick lil walk to clear my head.” Five days later, Nasca stopped at the Long Island Rail Road tracks that run through the hamlet of Bayport, New York, about half a mile from his house. He leaned his bike against a fence and stepped onto the track, at a blind curve his parents had warned him about since he was old enough to walk. He sent a message to a friend: “I’m sorry. I can’t take it anymore.” A train rounded the bend, and he was gone.
Bloomberg News, April 20, 2023
How parents can combat the ongoing teen mental health crisis
Recent data from the Centers for Disease Control and Prevention showed that three in five teen girls felt persistently sad or hopeless. It’s the latest troubling trend in an ongoing nationwide mental health crisis for teenagers.
Ishika Vij was just 12 years old when her anxiety started. After mounting pressure from schoolwork, Ishika developed an eating disorder.
“Just being able to control how I look versus, I thought, you know, I wasn’t worth enough or smart enough. So I was like, maybe I can be pretty enough or I can, you know, like follow these norms that, like, social media has set,” she said.
Sumeet Vij, Ishika’s father, said that his daughter’s generation is “different.”
“Their ability to cope with things is way different. They are resilient, but I think they are just exposed to a lot more things much earlier than we ever thought,” Sumeet Vij said.
Lisa Damour, a clinical psychologist and mother of two, said one way in which parents can combat this crisis is to limit their children’s access to social media.
“When girls are in distress they tend to collapse in on themselves, whereas when boys are in distress they tend to act out,” she said.
11-year-old who died after suicide attempt in N.J. school bathroom was bullied, mother says
Felicia LoAlbo-Melendez was found unresponsive in a bathroom stall at F.W. Holbein School in Mount Holly on Feb. 6 and died two days later.
An 11-year-old New Jersey girl who died days after an attempted suicide in a middle school bathroom had been relentlessly bullied and reported the harassment to school officials, her mother said.
The girl was found unresponsive in the bathroom stall at F. W. Holbein School in Mount Holly on Feb. 6 and died two days later, the Burlington County Prosecutor’s Office said.
Felicia LoAlbo-Melendez had been bullied for years, the girl’s mother, Elaina LoAlbo, said.
LoAlbo didn’t immediately respond to requests for comment Friday, but told NBC Philadelphia that her daughter was regularly taunted by classmates.
“They called her a furry. She was not a furry. They called her gay. They called her straight. They called her bi. They called her all kinds of things.”
“My daughter was being tortured within the walls of that school,” she added.
March 2023
Suicide can be contagious for teens, research shows. Here’s how parents can help
Tips on how to reduce the risk of suicide among teens from experts.
Rates of mental health emergencies are increasing among teenagers around the world, according to a new study from the University of Calgary. It found an increase in pediatric emergency room visits for suicide attempts, suicidal ideation, and self-harm during the first year of the pandemic.
It’s a particular concern because for teenagers, suicide can be contagious.
Teenagers with a friend or family member who died of suicide were at significantly higher risk of suicide than those without, according to a 2016 review published by the American Association of Suicidology.
Suicide Rates Start Spiking in Spring, This is Why and How to Get Help
Many people believe that suicide rates are at their highest during the winter months, specifically around Christmas, when many people struggle with loneliness, strains on their finances, and exacerbated family issues.
The truth in fact, is that the bulk of research consistently shows that the spring/summer months result in the highest number of suicides, a pattern that has remained consistent for many years. The Centers for Disease Control and Prevention reports that the highest number of suicides in the U.S in 2021 occurred in August. In fact, one study found that cardiac mortality is at its highest around Christmas and New Year’s than any other time of the year, making it far more of a risk factor than suicide at that time of year.
Screen Time Tied to Suicide Risk for Tweens – But Don’t Panic, Learn How Parents Can Help Kids Develop Safe Screen Habits
No one can blame parents for being spooked by new research finding that tweens’ risk of suicidal behavior increases with their amount of screen time. However, lead researcher Jason Nagata, MD, of UCSF Benioff Children Hospitals, says that caregivers should view these findings mostly as a reminder to ingrain healthy screen use habits in their kids as early as possible.
So your study found that screen use increases suicide risk?
The more time kids spend using screens from ages 9 to 11 years old, the higher their odds of suicidal behaviors two years later, at ages 11 to 13. Specifically, each additional hour of screen time increased the risk by 9%. The risk was highest with texting, followed by video chatting, watching videos, and playing video games. Social media didn’t show an effect, but that may be because, technically, kids aren’t allowed to be on social media platforms until they are 13 (though some still are), so we didn’t have as much data there.
University of California San Francisco, March 2, 2023
Black Children and Young Adult Suicide on the Rise
Suicide is an issue affecting people from all different cultures and backgrounds. But over the past few years, suicide rates have increased dramatically for black children and young adults between the ages of 10-24 years old.
For some time, mental health and suicide have been taboo in the black community, but with complex issues of racism, bullying, and generational trauma, Darryl Turpin, director of equity and cultural engagement for Lines for Life, a Portland suicide prevention agency, is trying to address the issue, by raising awareness about the unique reasons suicide is rising. This includes a lack of protective factors contributing to rising rates and the pressures of social media. Plus, Darryl reiterates that it will take the whole community being engaged in suicide prevention to help young people struggling with thoughts of suicide.
KXL 101 FM News, March 3, 2023
February 2023
Inside America’s youth mental health crisis: Kids in the U.S. and around the world are in crisis.
More than 60% of children with depression don’t get any mental health treatment, according to Mental Health America. Pair that statistic with the fact that about 80% of the United States has a severe shortage of child psychiatrists, and the picture becomes clear: there is a growing mental health crisis in the United States and beyond.
That’s why CBS News and local CBS-owned television stations spent more than six months exploring the sources of the problem, as well as solutions across the country that could address it. This is a collection of the reporting by CBS journalists, committed to the well-being of our kids.
Kids in the U.S. and around the world are in crisis.
More than 60% of children with depression don’t get any mental health treatment, according to Mental Health America. Pair that statistic with the fact that about 80% of the United States has a severe shortage of child psychiatrists, and the picture becomes clear: there is a growing mental health crisis in the United States and beyond.
That’s why CBS News and local CBS-owned television stations spent more than six months exploring the sources of the problem, as well as solutions across the country that could address it. This is a collection of the reporting by CBS journalists, committed to the well-being of our kids.
The New York Times, Feb. 27, 2023
CDC report: 30% of teenage girls say they have seriously considered suicide
It’s no secret that a mental health crisis is plaguing our children; a recent Centers for Disease Control and Prevention report highlighted concerning increases in sadness in teenage girls.
CBS2’s Christine Sloan investigated the alarming findings as parents desperately wonder what can be done.
That CDC report is painting a grim picture for teen girls in America, not only finding they’re facing record levels of sadness, but also they’re twice as likely as boys to take their own lives.
New Jersey high school student Adriana Kuch was just 14 when she died by suicide earlier this month.
“I look at Adriana and I see Mallory,” Dianne Grossman said. “Mallory was just a normal, everyday sixth grader. We used to say that she’s just the all-American little girl.”
Grossman says her daughter took her own life in 2017 at the age of 12, after being bullied at school for a year.
Teens Are Struggling Right Now. What Can Parents Do?
The psychologist Lisa Damour shares advice on how to connect, what healthy emotions look like and when to step in.
For over 25 years, the psychologist Lisa Damour has been helping teens and their families navigate adolescence in her clinical practice, in her research and in best-selling books like “Untangled: Guiding Teenage Girls Through the Seven Transitions Into Adulthood.”
This moment in time, she says, is like no other.
According to a report released last week by the Centers for Disease Control and Prevention, 42 percent of U.S. high schoolers experienced persistent feelings of sadness or hopelessness in 2021, while 22 percent seriously considered attempting suicide. Adolescent girls, as well as lesbian, gay and bisexual youth, are struggling the most, but boys and teens in every racial and ethnic group also reported worsening symptoms.
“I am deeply concerned about the suffering teens experienced during the pandemic and the current crisis in adolescent mental health,” Dr. Damour said.
In her new book, “The Emotional Lives of Teenagers,” Dr. Damour aims to demystify adolescence and to reset the very definition of mental health.
The New York Times, February 20, 2023
Bullying: How It Can Lead to Mental Distress, Suicide in Children
• Researchers say bullying can be a factor in mental distress and suicide attempts by children and teens.
• They say this type of distress is especially common among LGBTQ+ youth.
• Experts say parents can help children who are bullied by teaching them emotional and interpersonal skills as well as assisting them in building relationships with school personnel.
The reasons behind sadness, depression, and suicide among teens are complex, but some forms of bullying may play a role in increasing the likelihood of their occurrence.
That’s the conclusion reached in a study published today in the journal PLOS ONE.
Researchers say nearly one in three young people in the United States may experience bullying, with the occasional story of a teen’s suicide seemingly linked to bullying activity.
Teen Girls Report Record Levels of Sadness, C.D.C. Finds
Adolescent girls reported high rates of sadness, suicidal thoughts and sexual violence, as did teenagers who identified as gay or bisexual.
Nearly three in five teenage girls felt persistent sadness in 2021, double the rate of boys, and one in three girls seriously considered attempting suicide, according to data released on Monday by the Centers for Disease Control and Prevention.
The findings, based on surveys given to teenagers across the country, also showed high levels of violence, depression and suicidal thoughts among lesbian, gay and bisexual youth. More than one in five of these students reported attempting suicide in the year before the survey, the agency found.
The rates of sadness are the highest reported in a decade, reflecting a long-brewing national tragedy only made worse by the isolation and stress of the pandemic.
The New York Times, Feb. 13, 2023
How Do You Serve a Friend in Despair? by David Brooks
Over the years, Pete and I often spoke about the stresses he was enduring over the management of his medical practice, but I didn’t see the depths of what he was going through until we spent a weekend with him in the spring of 2019. My wife noticed a change immediately. A light had gone out; there was an uncharacteristic flatness in his voice and a stillness in his eyes.
One bright June afternoon, he pulled us aside and told us he wasn’t himself. He was doing what he loved most—playing basketball, swimming in the lake—but he couldn’t enjoy anything. He was worried for his family and himself and asked for our continued friendship and support. It was the first time I had seen such pain in him—what turned out to be severe depression. I was confronted with a question for which I had no preparation: How do you serve a friend who is hit with this illness?
I tried the best I could, but Pete succumbed to suicide last April. This article flows from what I learned from those agonizing three years and that senseless tragedy. It reflects a hard education with no panaceas.
The New York Times, Feb 9, 2023
When Schools Ask Students About Suicide, Those At Risk Get Help Sooner
It might, new research suggests.
Could asking teens a simple, but pointed, question about their mental health reveal whether they are at risk for suicide?
Since suicide is now the second leading cause of death among American teens, any strategy that could lower that risk may be worth trying.
“The depression screening tool we used is not a suicide risk assessment tool, but it does include one question that asks [students] about thoughts of self-harm,” explained study lead author Dr. Deepa Sekhar, an associate professor in the department of pediatrics at Penn State College of Medicine.
HealthDay, US News & World Report, February 3, 2023
Lack of Sleep Linked to College Student Suicide Risk
A new study identifies a link between sleep problems and suicidal thoughts, as well as behaviors that may help reduce suicide risk in young adults. In 2020, the Centers for Disease Control and Prevention reported suicide was the second leading cause of death among people ages 10-14 and 25-34, accounting for more than 9,000 deaths. Suicide also was the third leading cause of death among people ages 15-24, accounting for more than 6,000 deaths.
“Suicide is a difficult problem because it emerges from complex interactions between many, many different factors. Disrupted sleep is one such factor,” says Andrew Tubbs, a medical student researcher in the University of Arizona psychiatry department’s Sleep and Health Research Program.
“Our research shows poor sleep is linked with suicidal ideation, attempts, and deaths among college students. However, unlike other suicide risk factors, poor sleep isn’t permanent. If students can sleep better, maybe we can reduce suicide risk.”
How to Counter TikTok’s Mental Health Misinformation: The social media phenomenon is driving self-diagnosis.
“If you have inattention and rejection sensitivity, you may have ADHD,” says a vlogger to Clara one evening online. “When I get anxious, I zone out, and that’s how I know I have ADD,” says an influencer in the next video. Clip after clip, Clara is inundated with performers, experts, influencers, naturopaths, and everyone in between, highlighting an ADHD diagnosis or symptom on TikTok.
As one might imagine, Clara is confused. She is a 15-year-old with normal identity issues for her age but she has been socially isolated through her early adolescent years due to the pandemic. In trying to figure out and make sense of who she may be, her main source of information is the app known as TikTok. From it, she receives cues and hints about non-specific behaviors that offer her explanations as to how she interacts with the world.
Psychology Today, February 1, 2023
January 2023
Coping with The Teenage Suicide Epidemic
Suicide & drug overdose is at epidemic rates for teenagers. This article discusses what parents can do to help their teenager
Since the number of teenagers who are suicidal continues to increase, I decided to write this article for parents. Many parents ask me, if their child could be suicidal and what to do if their child is suicidal? This concern has increased since the CDC no longer ranks suicide as the third leading cause of death and now rates it as the second leading cause of death for kids 10 to 18 years old. Furthermore, since the quarantine for the Coronavirus there has been a significant increase in suicides and deaths from drug overdoses. As a result, parents are worrying more about if their teenager may be feeling suicidal.
Additionally, before the quarantine, parents were worrying more about suicidal teenagers as we learned more about suicides of survivors involved in mass shootings due to survivors dealing with survivor guilt. The issue of suicide is very scary especially because we do not discuss mental health issues in our society. As a result, parents are not sure what signs they should be looking for or what to do if they feel their teen is suicidal. Parents are aware there is a teenage suicide epidemic, but have no idea what to do or how to get help.
Patch, Pleasant Hill, CA, January 27, 2023
Social media’s effects on teen mental health comes into focus
Experts are increasingly warning of a connection between heavy social media use and mental health issues in children—a hot topic now driving major lawsuits against tech giants.
Why it matters: Seattle Public Schools’ recently filed lawsuit against TikTok, Meta, Snap and others—which accuses the social media giants of contributing to a youth mental health crisis— is one of hundreds of similar cases.
Driving the news: Some scientists who study technology’s effects on children say the negatives far outweigh any positives.
“There is a substantial link to depression, and that link tends to be stronger among girls,” Jean Twenge, a psychology professor at San Diego State University and leading expert on the subject, tells Axios.
“The more time the teen, particularly a teen girl, spends using social media, the more likely it is that she will be depressed,” said Twenge, whose book “iGen” describes how technology has shaped Gen Z.
The same is true for self-harm, Twenge said. “The more hours a day she spends using social media, the more likely she is to engage in self-harm behaviors — the link is there for boys as well, it’s just not as large.”
Suicide & Suicide-Related Outcomes Among Adolescents and Young Adults
Even though teen and young adult suicide is a persistent public health problem in the United States, the spatial patterns of suicide attempts and successful suicides are still, for the most part, a mystery. Another trend that is on the rise in this vulnerable demographic is nonfatal self-injury, which is considered a risk factor for suicide. Using data obtained from emergency departments, death certificates, and the violent death reporting system, researchers evaluate spatial clusters of cases of self-injury and suicide that occurred in the state of North Carolina between 2009 and 2018.
According to the findings, there is a startling disparity between the demographic profiles of individuals who deliberately take their own lives and those who inflict less severe types of self-injury. There was a distinct difference between where people killed themselves and where they hurt themselves intentionally. Micropolitan status, as well as measures of racial and income segregation at the area level, have the potential to be used to make predictions regarding clusters of high-risk suicides.
Physicians Weekly, January 16, 2023
Study Shows Correlation Between School Attendance and Suicide
What if schools are the major source of the youth mental crisisA lot of us likely remember the glee we felt as children at the onset of summer vacation, followed by the anxious anticipation of back-to-school time. For some children and teenagers, the start of a new school year generates intolerable levels of anxiety and depression. For a desperate portion of these young people, suicide seems like the only exit.
A new study, published this month by the National Bureau of Economic Research (NBER), finds a striking correlation between attendance in school and incidences of youth suicides. Analyzing several pre- and post-pandemic data sets, the researchers conclude “that youth suicides are closely tied with in-person school attendance.” According to the paper’s authors, youth suicides fall during the summer months and rise again when school begins. Notably, they found that in areas of the US where school begins in August, youth suicide rates also increase in August, while in areas that begin school in September, the youth suicide rate doesn’t increase until then.
This new study echoes earlier findings from Vanderbilt University researchers who discovered a similar link between school attendance and youth suicidal ideation and attempts. That research, published in the journal Pediatrics in 2018, looked at hospital emergency room and inpatient data between 2008 and 2015. “The lowest frequency of encounters occurred during summer months,” the Vanderbilt authors concluded. “Peaks were highest in fall and spring. October accounted for nearly twice as many encounters as reported in July,” they found
Catalyst Independent, January 3, 2023
December 2022
Teen Suicides Fell During Lockdown, Rose When In-Person Schooling Resumed, Study Finds
Suicide rates among teenagers fell sharply when schools were closed during the Covid-19 lockdown, but rose again when in-person schooling resumed, according to a new study.
Returning from online to in-person education was associated with an increase in the rate of teen suicides of as much as 18%.
The results provide convincing evidence that “in-person schooling is a contributor to teen suicide,” researchers say, with exposure to bullying likely to be a key factor in the link.
Schools around the world were closed to the vast majority of students from March 2020 as part of efforts to stop the spread of the pandemic.
But while there were concerns over the impact on children’s mental health of the disruption of their routines and enforced separation from their peers, suicide rates fell during lockdowns.
4 Genes May Raise Risk for Suicide
Scientists have pinpointed four genes that seem to play a part in how vulnerable you are to suicidal thoughts or behaviors.
“It’s important to note that these genes do not predestine anyone to problems, but it’s also important to understand that there could be heightened risks, particularly when combined with life events,” said study co-author Nathan Kimbrel. He’s an associate professor in the department of psychiatry and behavioral sciences at Duke University in Durham, N.C.
To find the culprit genes, Kimbrel and his colleagues conducted a large, genome-wide analysis using data from more than 630,000 U.S. military veterans. Participants were diverse, with 71.4% of European ancestry, 19.1% of African ancestry, 8.1% Hispanic and 1.3% Asian. Although most of the participants were men, 9% were women.
Medical records revealed more than 121,000 cases of suicidal thoughts or actions within that group. Those who had no documented lifetime history of self-harm behaviors were considered a control group.
Screening for the symptom of worthlessness could save your adolescent patient’s life…
New research finds that clinicians should ask routine questions about feelings of worthlessness at initial and follow-up examinations of adolescent patients with attention-deficit/hyperactivity disorder (ADHD) to help prevent suicide.
“We identified worthlessness and disorganized path of depression as the primary contributor to suicidal thoughts and planning,” wrote the authors.
Previous studies have found that ADHD, depression, and general anxiety disorder (GAD) are all strongly correlated with suicidal ideation. Specifically, adolescents with ADHD are at a higher risk of suicide than adolescents without ADHD.
The current study gathered 185 high school-aged children in Hungary, mean age of 14.79 years, with (N=89) and without (N=96) ADHD in order to assess the relationship between ADHD, depression, GAD, and worthlessness—a symptom experienced by 70% to 80% of patients with major depressive disorder.
Psychiatric Times, December 8, 2022
The Power of Connection: Suicide Prevention on Campus Feelings of hopeless and thoughts of suicide can touch anyone.
According to the Center for Disease Control and Prevention (CDC), suicide is currently the second leading cause of death among college students. The Healthy Minds Survey found that 14% of college students admit they had seriously considered suicide in the past year a figure that has doubled in the past decade. Since that figure just considers those that answered the survey chances are that figure is higher. Perhaps someone you know is silently struggling, trying to make it through the day push those thoughts aside. This is hope and there is help.
Although suicide can affect anyone, there are risk factors that make the likelihood increase. Childhood trauma, a mental health or substance abuse disorder, a family history of violence or abuse and stress are all contribute to an increased risk for suicide. Members of the LGBTQ+ community as well as African Americans also have greater risk of suicide. Being aware of the statistics alone means that you likely know someone who is suffering with suicidal thoughts. Knowing the warning signs is one way to help address this problem on your campus and community.
Young Americans increasingly end their own lives: Suicide is now the second-biggest killer of ten- to 18-year-olds
In the 1950s, when the term “teenager” was first popularised, it brought to mind trouble. Spotty youths who engaged in risky behaviour outside the house—getting drunk, pregnant or into car crashes—were “the number one fear of American citizens”, wrote Bill Bryson in his memoir, “The Life and Times of the Thunderbolt Kid”.
Today, the risks American teenagers face come from themselves. Boys are more likely to kill themselves than to be killed in a motor crash. Girls are nearly 50% more likely to injure themselves in a suicide attempt than to face an unplanned pregnancy. Suicide is the second-biggest killer of ten- to 18-year-olds, after accidents.
Identifying the Symptom of Worthlessness to Prevent Suicide in Adolescents With ADHD
New research finds that clinicians should ask routine questions about feelings of worthlessness at initial and follow-up examinations of adolescent patients with attention-deficit/hyperactivity disorder (ADHD) to help prevent suicide.
“We identified worthlessness and disorganized path of depression as the primary contributor to suicidal thoughts and planning,” wrote the authors.
Previous studies have found that ADHD, depression, and general anxiety disorder (GAD) are all strongly correlated with suicidal ideation. Specifically, adolescents with ADHD are at a higher risk of suicide than adolescents without ADHD. The current study gathered 185 high school-aged children in Hungary, mean age of 14.79 years, with (N=89) and without (N=96) ADHD in order to assess the relationship between ADHD, depression, GAD, and worthlessness—a symptom experienced by 70% to 80% of patients with major depressive disorder.
Psychiatric Times, December 8, 2022
November 2022
With Anxiety on the Rise, Some Children Try ‘Exposure Therapy’
A gold-standard treatment for phobias and anxieties encourages young people to follow an old and simple dictum: Face your fears.
One in 11 American children has an anxiety disorder, and that figure has been growing steadily for the past two decades. The social isolation, family stress and relentless news of tragedy during the pandemic have only exacerbated the problem.
Audrey Pirri, 16, had been terrified of vomiting since she was a toddler. She worried every time she shared a meal with family or friends, restricting herself to “safe” foods like pretzels and salad that wouldn’t upset her stomach, if she ate at all. She was afraid to ride in the car with her brother, who often got carsick. She fretted for hours about an upcoming visit to a carnival or stadium — anywhere with lots of people and their germs.
But on a Tuesday evening in August, in her first intensive session of a treatment called exposure therapy, Audrey was determined to confront one of the most potent triggers of her fear: a set of rainbow polka dot sheets.
For eight years she had avoided touching the sheets, ever since the morning when she woke up with a stomach bug and vomited on them. Now, surrounded by her parents, a psychologist and a coach in her pale pink bedroom, she pulled the stiff linens from her dresser, gingerly slid them over the mattress and sat down on top.
The New York Times, Nov. 27, 2022
Suicidal thoughts in kids were increasing likely long before the pandemic, study finds
Rates of ER visits and hospitalization among kids due to suicidal thoughts increased by almost 60% between January 2016 and mid-2021, a new study has found.
More and more kids are ending up in emergency rooms because they are contemplating suicide, a new study finds.
An analysis of Illinois emergency department data with national implications revealed that in fall 2019, there was a spike in visits from teens and younger children who were diagnosed as experiencing suicidal ideation. Researchers found another spike in fall 2020, according to the report published in Pediatrics on Nov. 14.
“One thing I want people to understand is that suicidal-ideation related emergency department visits were increasing before the pandemic,” said the study’s lead author, Dr. Audrey Brewer, an attending pediatrician at the Ann and Robert H. Lurie Children’s Hospital of Chicago.
Another important point, Brewer said, is that “during the pandemic we saw an influx of kids from all age groups. We tend to think about anxiety and depression as being common in older kids, but a lot of those who presented to the emergency department during the pandemic were between 5 and 13.”
How to talk to your teenagers about suicide, and what to do if they’re experiencing suicidal thoughts
Suicide is the second leading cause of death for ages 10-14, and the third for ages 15-19.
Asking a child directly about suicide can reduce their risk of dying by suicide.
If you are in crisis, text “HOME” to 741741 to reach the Crisis Text Line for immediate support.
Over the past 20 years, suicide rates in the United States have risen sharply. Currently, suicide is the second leading cause of death for teens ages 10-14, and the third leading cause of death for teens ages 15-19.
Not everyone is at equal risk: Teens involved in the juvenile justice and child welfare systems, LGBTQ+ teens, Native American and Alaskan Native teens, and teens currently or formerly involved with the military could all be at higher risk of attempting or dying by suicide.
It’s important for parents or caregivers of loved ones to identify signs of suicide or suicidal ideation as soon as possible so they can get their kids help, says John Seeley, a professor in the School of Education at the University of Oregon.
October 2022
Needs matter: Factors that increase suicide risk for college students
Regardless of sociodemographic background, college students across the country struggle with suicidal thoughts and behaviors. According to the Centers for Disease Control and Prevention, suicide was one of the top nine leading causes of death for people in 2020.
Yusen Zhai, Ph.D., assistant professor of counseling in the University of Alabama at Birmingham’s School of Education and director of the UAB Community Counseling Clinic, emphasizes the importance of building awareness of suicide and ways to prevent suicide.
In a recently published paper, Zhai and his co-author looked at trends and prevalence of suicide among college students in the United States during the COVID pandemic. The research found that students who struggle with food insecurity are at elevated risk for suicide.
3 Out of 4 Teens Reported Adverse Event that Puts Them at Risk for Poor Mental Health
• About 37% of teens surveyed by the CDC reported poor mental health during 2020.
• At least 73% reported at least one adverse childhood experience (ACE).
• ACEs are associated with an increased risk of mental health problems and an increase in suicidal thoughts.
Many people have reported concern about the effects of COVID on mental health. Teenagers in particular have been affected after dealing with social distancing and missing in-person school. Additionally, many faced traumatic events during the pandemic.
Now the CDC has recently released a report about the COVID-19 pandemic and adolescents’ mental health. About 37% of those surveyed reported poor mental health during 2020. At least 73% reported at least one adverse childhood experiences (ACEs) during that time, and 12% experienced three or more.
Those who had experienced ACEs were more likely to report mental health problems and suicide attempts than those who did not.
Too Few Young People Get Mental Health Follow-Up After ER Visit
When teens and young adults go to the emergency room or are hospitalized for critical mental health issues a staggering number are not receiving quick follow-up care, new U.S. research finds.
Researchers at the University of Massachusetts looked at more than 100,000 ER visits of young people ages 12 to 27 who have private insurance. Only about 29% received follow-up care within seven days after their crisis. Less than half–just 46%–received follow-up care within that first month.
Similarly, in 95,000 youths and young adults whose cases were so severe they were hospitalized, less than 43% had after care within seven days and 67% within 30 days.
That left many young people without professional help while still vulnerable, including to risk of suicide.
Consumer Health Day, Oct. 17, 2022
Teen Suicides Jump 29% Over the Past Decade, Report Finds
Nevada saw the biggest increase; American Indian/Alaska Native teens most vulnerable overall.
Suicides jumped 29% among adolescents ages 15 to 19 over the previous decade, according to a report released Wednesday.
Adolescent suicides rose from 8.4 per 100,000 during the 2012-2014 timeframe to 10.8 deaths per 100,000 in 2018-2020, according to the new edition of America’s Health Rankings Health of Women and Children Report from the United Health Foundation. Adolescent suicides also rose significantly in 10 states. The report captures 121 health measures based on the most recently available public health data from 30 different sources.
On a state-by-state basis, Nevada, Colorado, and South Carolina saw the greatest relative increases in teen suicides during the time periods studied:
• Nevada: 82% increase (8.3 to 15.1 per 100,000)
• Colorado: 67% increase (12.9 to 21.5 per 100,000)
• South Carolina: 55% increase (8.7 to 13.5 per 100,000)
September 2022
Suicides are spiking among young men: The suicide rate is nearly back up to the 2018 all-time high
The nation’s suicide rate in 2021 increased for the first time in two years with the largest spike seen among males ages 15-24.
The provisional data released today shows a 4 percent rise in suicides last year. It comes as the country is still contending with the aftereffects of covid-19 disruptions and amid calls for officials to address a growing mental health crisis.
The Centers for Disease Control and Prevention didn’t speculate on what’s behind the increase, and the causes of suicide are complex, often determined by multiple factors. Those can consist of depression, family history of suicide, physical illness, childhood trauma and more.
Experts also pinpointed issues that might aggravate that risk, such as a rise in guns in the home, loss of jobs and loved ones amid the pandemic, last year’s covid-19 spike and the influence of social media on teens, our colleague Lenny Bernstein reports.
The Washington Post, Sept. 30, 2022
Can Smartphones Help Predict Suicide?
A unique research project is tracking hundreds of people at risk for suicide, using data from smartphones and wearable biosensors to identify periods of high danger — and intervene.
In March, Katelin Cruz left her latest psychiatric hospitalization with a familiar mix of feelings. She was, on the one hand, relieved to leave the ward, where aides took away her shoelaces and sometimes followed her into the shower to ensure that she would not harm herself.
But her life on the outside was as unsettled as ever, she said in an interview, with a stack of unpaid bills and no permanent home. It was easy to slide back into suicidal thoughts. For fragile patients, the weeks after discharge from a psychiatric facility are a notoriously difficult period, with a suicide rate around 15 times the national rate, according to one study.
This time, however, Ms. Cruz, 29, left the hospital as part of a vast research project which attempts to use advances in artificial intelligence to do something that has eluded psychiatrists for centuries: to predict who is likely to attempt suicide and when that person is likely to attempt it, and then, to intervene.
The New York Times, Sept. 30, 2022
“You’re not alone”: Suicide attempts among teen girls increased 50% during pandemic, CDC finds
Bethlehem, Connecticut — Emma Wanstall has learned it’s OK to ask for help. The 18-year-old former cheerleader started treatment for her mental health in July after she fell into a deep depression during the pandemic.
“It got to the point where I overdosed,” she said. “I was planning on going to bed that night and not waking up in the morning.”
At first, Wanstall struggled opening up to her parents about her mental health, saying she felt like it would “make them feel they failed as a parent.”
Suicide is the third leading cause of death among people aged 15 to 24 in the U.S., according to the Centers for Disease Control and Prevention. Since 2019, the number of teenage girls who have been suicidal has increased 50%, according to the CDC.
Samantha Quigneaux, a family therapist at Newport Healthcare, said it’s getting worse because of “the pressure of the return to normalcy.”
CBS Evening News, Sept. 23, 2022
Higher Risk of Suicide Observed in Adolescents Suffering from Nightmare Distress
Insomnia, Nightmares & Depression in Adolescents: Experiencing a nightmare is a common phenomenom, particularly among the general adolescent population. Various consequences have been linked to nightmares and can have a severe impact on mental health, even leading to increased risk of suicide.
The experience has been characterized as dysphoric, frightening, or disturbing dreams that can inflict intense irritability and lead to disrupted sleep. As the prevalence of nightmares experienced by an individual increases, so does their vulnerability for insomnia, daytime sleepiness, anxiety and depressive symptoms, post-traumatic stress disorder (PTSD), behavioral problems, and impaired psychosocial function.
While previous evidence has shown that adults with major depressive disorder (MDD), bipolar disorders, or schizphrenia encounter this dysphoric dream state more frequently than the general population, there’s a lack of evidence when it comes to adolescents with MDD.
HCPLive Network, Sept. 23, 2022
August 2022
‘The Best Tool We Have’ for Self-Harming and Suicidal Teens
Studies indicate that dialectical behavior therapy offers greater benefits than more generalized therapy. But treatment is intensive, and expensive.
Parents seeking therapy for teenagers who self-harm or suffer from anxiety, depression or suicidal thoughts face an imposing thicket of treatment options and acronyms: cognitive behavioral therapy (C.B.T.), parent management training (P.M.T.), collaborative assessment and management of suicidality (CAMS), acceptance and commitment therapy (ACT) and others.
Each approach can benefit a particular subset of people. But for teenagers at acute risk for self-harm and suicide, health experts and researchers increasingly point to dialectical behavior therapy, or D.B.T., as an effective treatment.
“As of this moment, it’s probably the best tool we have,” said Michele Berk, a child and adolescent psychologist at Stanford University.
The New York Times, August 27, 2022
Children’s Risk of Suicide Increases on School Days
Unlike in adults, suicide risk among children is lowest during the summer and higher during the school year. Understanding these patterns can help prevent and treat suicidality.
Pediatricians, child psychologists and psychiatrists, social workers and pediatric emergency teams know something that many people who care for children don’t: we are much busier during the school year. I’m a full-time emergency psychiatrist who works at a major children’s hospital, and often when children come in for a mental health crisis, one of the main stressors they discuss is school.
I’m sure most people assume I commonly prescribe medications as a physician, but one of my most common “prescriptions” is advocating for reducing school burden and load. In a 2013 American Psychological Association survey, 83 percent of adolescents stated that school was a cause or significant source of stress.
Scientific American, August 22, 2022
How easy access to guns at home contributes to America’s youth suicide problem
School shootings in the U.S. are national tragedies, and the toll they take in lives cut short and traumatized distinguishes the U.S. from other high-income countries. But there is another way that guns are killing American children, and in far greater numbers: suicide.
Between 2011 and 2020, the most recent decade for which data is available, 14,763 children ages 5-17 died by suicide in the U.S. – a rate of approximately four deaths every day. Over 40% of these suicides involved a firearm. The great majority of guns involved in youth suicides come from the victim’s home or the home of a relative.
As scholars who have studied firearm violence and suicide prevention, we know the exceptionally high rate of gun suicides by U.S. youths is directly linked to the easy access many young people have to guns in and around the home.
The Conversation, August 17, 2022
Youth mental health is in crisis. Are schools doing enough?
For fourth-grader Leah Rainey, the school day now begins with what her teacher calls an “emotional check-in.”
“It’s great to see you. How are you feeling?” chirps a cheery voice on her laptop screen. It asks her to click an emoji matching her state of mind: Happy. Sad. Worried. Angry. Frustrated. Calm. Silly. Tired.
Depending on the answer, Leah, 9, gets advice from a cartoon avatar on managing her mood and a few more questions: Have you eaten breakfast? Are you hurt or sick? Is everything OK at home? Is someone at school being unkind? Today, Leah chooses “silly,” but says she struggled with sadness during online learning.
At Lakewood Elementary School, all 420 students will start their days the same way this year. The rural Kentucky school is one of thousands across the country using the technology to screen students’ state of mind and alert teachers to anyone struggling.
The Concerns Looming Over The 988 Mental Health Hotline
Dialing for help in a mental health crisis just got shorter. Now, Americans can dial 988 for assistance in an emergency instead of a previous 10-digit number directing them to the national suicide prevention hotline.
The Biden administration is giving local call centers $432 million to beef up support via additional staffing and Spanish-speaking agents.
Some concerns have emerged during the service’s rollout. There are questions about how centers will continue to fund these efforts long-term after the initial funding runs dry. Questions about police intervention have mounted, especially in the queer and Black communities.
$5.3 Million in Grants Awarded to Address Youth Mental Health Crisis
Inaugural recipients will use funds to support infrastructure, student mental health, and programs for children with behavioral challenges.
Three organizations dedicated to helping address the youth mental health crisis in the United States will be awarded $5.3 million in grants.
The inaugural recipients include The Jed Foundation, the National Alliance of Healthcare Purchaser Coalitions’ Path Forward initiative, and the Think:Kids & Meadows Mental Health Policy Institute (MMHPI) partnership.
The Jed Foundation, which focuses on emotional health support and suicide prevention for adolescents and young adults, plans to use the grant funds to create more partnerships with high schools, colleges, and universities in support of student mental health.
“We are extremely grateful to receive The Goodness Web’s inaugural grant that fortifies and expands our ability to increase our programming to support youth mental health and suicide prevention nationwide,” said JED CEO John MacPhee in a press release.
“Our goal is to partner with more than half of the country’s colleges and universities and more than 1000 high schools to implement a mental health culture of caring that improves well-being and reduces risks for suicide for their more than 13.2 million students.”
Psychiatric Times, August 8, 2022
Suicide Rate Is Spiking Upwards in Preadolescent Children
In the past two decades, a growing number of preteens have taken medicines or other chemicals as a way to end their lives, new research warns.
The mental health of children has become a big talking point in light of the pandemic, but the study data showed the problem has been percolating for years: There has been a 4.5-fold increase in suicidal ingestion cases among children between the ages of 10 and 12 since 2000.
Study co-author Dr. David Sheridan, a pediatric emergency room doctor at Oregon Health and Science University, said mental health concerns are a growing issue in emergency department patients.
“We’ve just seen rapidly escalating numbers of adolescents coming in with suicidal thoughts. And it seems like we’ve been seeing younger patients as well,” Sheridan said.
To verify this anecdotal information, the researchers turned to data collected in the National Poison Data System for children aged 6 to 18. The cases were coded to show whether it was a suspected suicide attempt or recreational misuse or abuse of a drug or chemical, as well as the final outcome in each case.
Consumer Healthday, August 8, 2022
July 2022
If the Kids are Not All right, Neither are Working Caregivers
By now we’ve all seen the headlines about the youth mental health crisis. We’ve likely even seen the effects in our own families, whether from the ongoing impact of social isolation, or from anxiety, depression, and trauma induced or exacerbated by the spate of gun violence and racial violence in our communities.
While roots of the pediatric mental health crisis existed well before the pandemic, rates of clinical anxiety and depression among youth have doubled in the past two years. And suicide-related mortalities among children and adolescents are rising at an alarming rate. New legislation, from anti-LGBTQ+ laws to barriers to abortion access, continue to fuel this mental health crisis among teens and families.
It’s critical to act now to support children and families in the midst of the “hidden” pandemic that we’re experiencing: the youth mental health crisis. We must do so not only to help our kids become healthier and happier but also to maintain the health of corporate America.
Everything to know about the new crisis hotline, 988
A new three-digit dialing code, 988, has been designated to route calls and texts to the National Suicide Prevention Lifeline. It launched over the weekend, on July 16.
The hotline, whose existing number will remain in operation, will expand to help callers more broadly in emotional distress. The launch has been funded in part by Health and Human Services.
“What’s been really cool out of this is actually that a lot of the states have used the funding to implement mental health crisis response teams,” vice president of clinical operations for NeuroFlow Matt Miclette, R.N., told Fierce Healthcare. NeuroFlow offers tech-powered engagement tools for providers, including a platform that will show the 988 number in two separate places for patients.
In the past, NeuroFlow had to work with law enforcement to respond to emergency situations. Now, many states are enacting legislation related to 988 like establishing mental health crisis response teams for referrals instead. “The best thing about that is we’re limiting the amount of police encounters,” Miclette said.
Fierce Healthcare, July 18, 2022
Change of National Suicide Prevention Lifeline Number to 988
“The need for quick, easy, and reliable access to emotional support and crisis counseling in the United States has never been greater. The COVID-19 pandemic laid bare the stressors faced by Americans. Too often, such stressors result in suicidal and mental health crises,” said Tom Coderre, acting assistant secretary for mental health and substance use and the interim head of the Substance Abuse and Mental Health Services Administration (SAMHSA). This is why the National Suicide Prevention Lifeline (1-800-275-TALK (8255)) change to 988 cannot come at a more opportune time.
According to Hannah Collins, Director of Marketing and Communications at Vibrant Emotional Health, the administrator of the National Suicide Prevention Lifeline, a direct 3-digit line to trained counselors can open the door for millions of Americans to seek the help they need, while sending the message to the country that healing, hope, and help are happening every day.
Psychiatry Advisor, July 8, 2022
Young people’s mental health is getting worse but mindfulness training isn’t the answer, large UK study suggests
There is a crisis in teen mental health, and schools in many countries are exploring different ways to make young people more resilient.
However, a UK-based research project, the largest of its kind on the subject, has suggested mindfulness training in schools might be a dead end — at least as a universal, one-size-fits-all approach.
The study, which involved 28,000 children, 650 teachers and 100 schools, looked at the impact of mindfulness training over an eight-year period and found that the technique didn’t help the mental health and well-being of adolescents ages 11 to 14. The authors suggested investigating other options to improve adolescent mental health.
“Adolescence is an absolutely crucial time of development,” said Willem Kuyken, the Sir John Ritblat Family Foundation Professor of Mindfulness and Psychological Science at the University of Oxford and one of the lead researchers involved in the project. “The brain goes through important and fundamental changes in adolescence that set the trajectory for people’s lives.”
Debunking myths about suicide helps encourage compassion and understanding
Sometimes people who die by suicide get branded as selfish, depressed or attention-seeking.
Such myths contribute to the stigma that can prevent those who are suicidal from seeking the help they need and falsify understanding of the motivations behind suicide, according to the National Alliance on Mental Illness, or NAMI.
Suicide is a leading cause of death among children and adults, with nearly 800,000 people worldwide dying from suicide yearly, according to the Global Burden of Disease Study 2017, cited by the online scientific publication Our World in Data. In 2020, there were 1.2 million attempts globally, the American Foundation for Suicide Prevention says.
People considering suicide might show signs early on. Here’s what to watch for
Awareness of the realities of suicide can help people view these deaths with more understanding and compassion, realize the importance of helping others get help and address their own mental health problems if they are struggling, NAMI says.
Before Heading to College, Make a Mental Health Checklist
Students should not wait until they are on campus to begin thinking about how to protect their emotional well-being, experts
As fall approaches, new students will arrive on college campuses toting all kinds of things: luggage and school supplies, mini fridges and sports equipment. But in the midst of the preparation for move-in day, many have not considered what tools they will need to support themselves emotionally.
In other words, what can they do to protect their mental health?
In a 2017 survey of more than 700 parents and guardians, over 40 percent said they did not discuss the potential for either anxiety or depression when helping their teenagers prepare for college or postsecondary school. In addition, most of the caregivers said mental health services on campus were not a priority when choosing a school.
But a large number of teenagers are struggling. According to the Centers for Disease Control and Prevention, more than 1 in 3 high school students experienced persistent feelings of sadness or hopelessness in 2019, representing a 40 percent increase since 2009.
The New York Times, July 8, 2022
June 2022
AAP Blueprint for Youth Suicide Prevention: A Roadmap
In February of 2021, the AAP, NIMH, and the AFSP convened, along with over 100 clinicians, a workgroup with a shared goal and dream of compiling a roadmap for youth suicide prevention, and in March of 2022, the AAP Blueprint for Youth Suicide was released.
This comprehensive body of work provides clinical pathways, initiatives for community partner collaborations, resources, and advocacy materials. Additionally, there is an extensive section on the epidemiology of youth suicide informed by a health equity lens. The panelists share the story of the creation of the Blueprint along with practical information on the navigation of the site.
Today we are joined by Dr. Lisa Horowitz, Dr. Christine Moutier, and Dr. May Lau
Pediatric Meltdown with Lia Gaggino, podcast
New Data Reveals Massive Spike in Self-Harm, Suicide Calls Among Adolescents
The Washington Poison Center analyzed call data between 2019 and 2021 and found that reports of self-harm and suicide by adolescents jumped by 58 percent.
June 16, 2022 – While reviewing data from the peak of the COVID-19 pandemic, researchers from the Washington Poison Center (WAPC) found that there was a substantial increase in reports of self-harm and suicide among the adolescent population.
Operating since 1956, WAPC is a nonprofit organization that assists residents of Washington state with calls related to poisoning and toxic exposures. WAPC also helps public policymakers and health leaders by providing resources that display public health trends.
While reviewing calls made to the center from 2019 to 2021, WAPC researchers reported that the increase in suicidal adolescents, a trend that began before the pandemic, continued. Within this three-year period, there was a 58 percent increase in 6 to 12-year-old patients reporting suicidal thoughts.
Health IT Analytics, June 16, 2022
Out of the Darkness Overnight Walk for suicide prevention kicks off from Intrepid Museum
Hundreds of people are took part in an overnight walk in Manhattan in the fight against suicide.
The Out of the Darkness Overnight Walk kicked off from the Intrepid Museum on the West Side on Saturday night.
As CBS2’s Vanessa Murdock reported, the walk takes place in one night with one goal — stop suicide.
The cause is especially important for CBS2’s Cindy Hsu.
“I attempted suicide seven years ago, and there are so many people who are suffering from mental illness in silence, and so we need to talk about depression and bipolar and everything else and just normalize it because we’re not alone,” Hsu said.
Saturday night’s walk was a testament to that. Hsu along with 1,800 others whose lives have been affected by suicide walked 18 miles. Some wore t-shirts to remember those lost. Many wore honor bead symbolizing why they walk.
Hsu was the honor bead ceremony speaker and participated in the walk, wearing green beads to symbolize a personal struggle.
“My godbrother and I lost somebody that I love,” said Roland Brown, of Cambria Heights.
Firearm suicide among America’s youth has hit its highest rate in 20 years, report finds
As the debate over gun policy has once again moved to the forefront following a string of mass shootings, a new report by Everytown for Gun Safety is shedding light on another aspect of gun violence impacting children: suicide.
The report, published on Thursday, found that the rate at which children, teens and young adults are dying by suicide by use of a firearm has increased faster than any other age group over the past decade. According to the group, firearm suicide among ages 10 to 24 is at its highest rate in more than 20 years.
From 2019 to 2020 alone, while the rate of firearm suicides increased by 2% as a whole, the rate among ages 10 to 24 increased by 15%.
A Growing Number of Young People Are Attempting Suicide by Self-Poisoning
Suicides among young people have been on the rise for a long time. Among 10 to 24 year olds, overall rates of deaths by suicide in the U.S. increased 57% from 2000 to 2018, according to federal data. Now, a new study published in the journal Clinical Toxicology has looked more closely at a particular method of attempted suicide—self-poisoning—and turned up some disturbing results: From 2015 to 2020, suicide attempts by ingesting toxic substances or overdosing on medications soared by 26% among people ages 6 to 19.
The research, led by Dr. Jennifer Ross, a medical toxicologist at the University of Virginia School of Medicine, relied on figures from the National Poison Data System, which aggregates information from the country’s 55 state and territorial poison control centers. From 2015-2020, there were 514,350 calls to poison control centers involving children ages 6-19 who, according to the control centers’ guidelines for suspected suicide attempts, had “an exposure resulting from the inappropriate use of a substance for self-harm or self-destructive” reasons.
May 2022
Families of college students who died by suicide unite for ‘powerful moment’ of healing
College suicide is a leading concern among mental health experts. Families who lived through it share their stories.Families with a shared nightmare — the death of their college students through suicide — hope their stories can prevent more loss.
On Tuesday, the parents of college athletes Katie Meyer, Arlana Miller, Morgan Rodgers and Tyler Hilinski spoke to TODAY about the legacy of their children.
“It’s a powerful moment for all of us to be together,” Gina Meyer, the mother of Katie, tells NBC correspondent Stephanie Gosk on TODAY.
Gina and Steven Meyer’s 22-year-old daughter was a soccer goalie at Stanford University in California, where she studied international relations and history. In March, Katie died of suicide.
At the time, Gina told NBC News that the “horrific” ordeal was “a parent’s worst nightmare” and there were “no red flags” about their daughter’s mental health. Still, her parents have wondered whether Katie struggled under academic and sports commitments.
Although there are risk factors for suicide (substance abuse, depression, anxiety disorders are several listed by the American Foundation for Suicide Prevention), experts say there aren’t clear warning bells. As Julie Cerel, a licensed clinical psychologist at the University of Kentucky previously told NBC News, “Suicide doesn’t discriminate.”
According to the Centers for Disease Control and Prevention, suicide is the second leading cause of death for people between the ages of 10 and 34.
Prevalence of preteen suicide has more than doubled in 11 years: ‘Concerningly high’
The fifth leading cause of death among preadolescents
The prevalence of preteen suicide has more than doubled in 11 years, an alarming trend that researchers say needs urgent study in order to prevent such tragedies.
In 2008, suicide was the 10th leading cause of death among preadolescents, according to the Centers for Disease Control and Prevention. By 2019, the most recent year for which statistics were available, it was the fifth, causing the National Institute of Mental Health to identify it as a priority for research and intervention.
“To me, that just seemed concerningly high, especially considering their age,” said Richard Liu, an associate professor of psychology at Harvard Medical School and one of the authors of a new article on the subject in JAMA Psychiatry.
Although a substantial number of studies have focused on self-injurious thoughts and behaviors (SITBs) in adolescents and adults, the amount of research on SITBs in children 12 or younger is slim, Liu and his co-authors found.
In the case of suicidal thoughts and behaviors, this is due in part to the long-held belief that preadolescent children don’t have the cognitive capability to understand the nature of death — and so they’re incapable of thoughts or acts of suicide.
“If a child says they’re going to kill themselves, quite often people say, ‘Oh, they don’t really mean what they’re saying,’” said Liu, director of suicide research in the Division of Child and Adolescent Psychiatry at Massachusetts General Hospital. “It’s just hard to fathom children that young having these kinds of thoughts and experiences.”
Young Advocates Lead Effort to Curb Campus Suicide
When the campus alert system at the University of California at Los Angeles notified students of a possible shooter this February and directed them to shelter in place, senior Meera Varma found herself surrounded by frightened students.
She told the alarmed undergrads hunkered down in the dorm it was OK to be scared – a technique she’d learned in a mental health training.
“Residents told me they were really nervous, they didn’t know what to do,” said Varma, a resident advisor at the dorm.
“I validated their feelings and told them you’re not alone in feeling scared. I told them I appreciated that they trusted me and wanted to come to me.” She then assured them that she could refer them to the counseling center once the danger was over.
The tool that Varma used, which goes by the acronym VAR – Validate, Appreciate, Refer – was created by a national mental health organization for students called Active Minds. The group teaches thousands of students the crisis intervention technique each year in 600 campus chapters.
Center on Media Crime and Justice at John Jay College, May 23, 2022
Are TikTok Algorithms Changing How People Talk About Suicide?
Social media users have adopted terms like unalive to avoid platform censorship. But not using the word suicide can stigmatize it. KAYLA WILLIAMS HAS never said the word “suicide” on TikTok, even though she uses the platform to discuss mental health issues with her 80,000 followers. Since the beginning of the pandemic, the 26-year-old student from Berkshire, England, has posted multiple videos about suicidal ideation and her stay in a psychiatric ward.
Some of these clips are lighthearted, others far more serious. Yet Williams does not utter the word “suicide” to her front-facing camera, or type it in her captions, for fear the TikTok algorithm will censor or remove her content. Instead, she uses the word “unalive.”
The hashtag #unalivemeplease has 9.2 million views on TikTok; #unaliving has 6.6 million; #unaliveawareness has an additional 2.2 million. Though #suicideprevention is a frequently used tag on the app, the hashtags #suicide and #suicideawareness do not exist—if you search for them, TikTok pulls up the number for a local crisis helpline. It’s a well-intentioned policy, initiated in September 2021, a year after a graphic video of a suicide spread across the app.
But users have also come to fear elusive content moderation filters that seemingly suppress or remove videos discussing death, suicide, or self-harm.
Guns in the Home Raise Suicide Risks for Teens
Teens who have access to guns are at a higher risk for suicide or suicide attempts, new research shows.
Compounding the situation, about one-third of all U.S. adolescents coming to the emergency department for any reason have moderate or severe depressive symptoms, suggesting high mental health needs among this population, the study authors said.
And more than 40% of those depressed teens have access to a gun, the researchers found.
“Our findings underscore the importance of screening all adolescents who present to the emergency department for suicide risk and access to firearms,” said lead study author Dr. Samaa Kemal. She is a pediatric emergency medicine fellow at Children’s Hospital of Chicago. “This is even more critical now that we are in the midst of a youth mental health crisis.”
Teens and preteens with access to guns had about 1.5 times higher odds for a prior suicide attempt or current suicidal ideation, the study found. And this was prior to the pandemic, when emergency departments saw increased youth mental health needs.
U.S. News and World Report, May 26, 2022
Preteen Suicide a ‘Worrying Trend,’ and Research Is Lacking—15% of preteens have thoughts of suicide, according to meta-analysis
While deaths by suicide among preteens are rare, they are increasing, and self-injurious thoughts and behaviors are occurring with “concerning frequency,” according to a systematic review and meta-analysis.
Among over 600 million individuals across 58 studies, the lifetime prevalence of suicide was 0.79 per 1 million children across the general population, and pooled prevalence estimates for suicidal ideation, suicide attempts, and nonsuicidal self-injury were 15.1%, 2.6%, and 6.2%, respectively, among community samples, reported Richard Liu, PhD, of Massachusetts General Hospital and Harvard Medical School in Boston, and colleagues.
In addition, approximately 17% of preteens who have suicidal thoughts will later attempt suicide, they noted in JAMA Psychiatry.
“Roughly one in a million children will end up dying by suicide,” Liu told MedPage Today.
Predictors of bullying, depression, and suicide attempts among youth: The intersection of race/ethnicity by gender identity
Highlights
• Understanding intersectionality of race and ethnicity and gender identity and its significant association with different health-related risks among youth.
• Reveal higher risks for youth with multiple marginalized identities; Specifically, youth identifying both as Multiracial and as transgender/non-binary had significantly higher levels of depression and suicidal ideation compared to cisgender White youth.
• Provided ideas about developing prevention and interventions that use intersectional approaches in practice and school environment.
CDC: 64.1 Percent of Violent Deaths in 2019 Were Suicides
In 2019, most violent deaths were suicides, which occurred more often in males than females, according to research published in the May 20 issue of the U.S. Centers for Disease Control and Prevention Morbidity and Mortality Weekly Report.
Rebecca F. Wilson, Ph.D., from the CDC in Atlanta, and colleagues analyzed data from the CDC National Violent Death Reporting System for 50,374 fatal incidents involving 51,627 violent deaths that occurred in 42 states and the District of Columbia in 2019.
Evaluation of Suicides Among US Adolescents During the COVID-19 Pandemic
In 2021, the American Academy of Pediatrics declared a state of emergency regarding child and adolescent mental health.1 During the COVID-19 pandemic, US adolescents have been affected by the widespread loss of primary caregivers. Suicide-risk screenings have yielded higher positive rates than during the prepandemic period2; thus, we sought to measure suicide-related mortality in this population.
These findings highlight the importance of alleviating the downstream consequences of the pandemic for adolescent well-being. Examples of interventions that may address shifting suicidality among young people in the US include expanding bereavement counseling to cope with the loss of caregivers and implementing more readily available suicide risk assessment solutions.
Are the Kids All Right? How Series Can Better Represent Teen Mental Health on Screen
The subject of teenage depression is generally played for high-octane drama in showbiz. In 2017, “13 Reasons Why” fell under rapid-fire controversy for its inclusion of a graphic suicide scene, which was ultimately removed by Netflix. Conversely, in Hulu’s true crime miniseries “The Girl From Plainville,” the pinnacle suicide scene is kept off-camera. And then there’s “Euphoria,” HBO’s Emmy-winning, millennial-targeted juggernaut charting the disease of addiction in Rue (Zendaya), whose rampant substance abuse-cum-debilitating anxiety is punctuated by police chases, drug lords and toxic teenage love triangles.
But depression isn’t always — or even most of the time — the stuff of season-ending cliffhangers. It’s dull, weighty. It is as heavy as a rock chained to one’s ankle. In the United States, rates of adolescent depression have climbed to epidemic proportions.
Per the Centers for Disease Control and Prevention, 13% of adolescents reported having a major depressive episode in 2019, a 60% jump from 2007. In 2018, suicide rates for people ages 10-24 also leapt 60%. Suicide is a leading cause of death among youth ages 10 to 19 years.
Given this catastrophic trend and in May, dubbed Mental Health Awareness month, Hollywood should consider normalizing its depiction of mental illness, centering (at least some) stories on the millions of adolescents who cope with clinical depression.
Morgan will be 22 forever. How pressure of college sports can harm athletes’ mental health.
Push through it. Tough it out. Suck it up. Shake it off. Calm down. Let’s go, let’s go!
And, of course, there’s “snap out of it.”
Those last four words may have worked well for Cher and Nicolas Cage in “Moonstruck,” but it’s just another troublesome phrase to high school and collegiate student-athletes when they are struggling to balance their mental health with the demands of academics, social life and excelling in competitive sports – training, conditioning, practice, travel and games.
Whether it’s challenging phrases, team culture, personal expectations or the self-imposed pressure to perform at a high level, “elite” athletes are expected to adapt and control their circumstances. Anything less is, well, not acceptable.
For some, the anxiety, depression or other pressures become unbearable, and tragically another athlete dies by suicide.
Hundreds of Suicidal Teens Sleep in Emergency Rooms. Every Night.
On a rainy Thursday evening last spring, a 15-year-old girl was rushed by her parents to the emergency department at Boston Children’s Hospital. She had marks on both wrists from self-harm and a recent suicide attempt, and earlier that day she confided to her pediatrician that she planned to try again.
At the E.R., a doctor examined her and explained to her parents that she was not safe to go home.
“But I need to be honest with you about what’s likely to unfold,” the doctor added. The best place for adolescents in distress was not a hospital but an inpatient treatment center, where individual and group therapy would be provided in a calmer, communal setting, to stabilize the teens and ease them back to real life. But there were no openings in any of the treatment centers in the region, the doctor said.
Indeed, 15 other adolescents — all in precarious mental condition — were already housed in the hospital’s emergency department, sleeping in exam rooms night after night, waiting for an opening. The average wait for a spot in a treatment program was 10 days.
The girl and her family resigned themselves to a stay in the emergency room while she waited. But nearly a month went by before an inpatient bed opened up.
The New York Times, May 8, 2022
Some States Back Away From a Major Student Well-Being Survey. Why, and What It Could Mean
As schools face a student mental health crisis, some experts fear that a growing resistance to collecting data about child well-being could jeopardize key efforts to protect kids.
Florida officials notified the Centers for Disease Control and Prevention in March that the state would no longer administer an anonymous, voluntary, biennial survey centered on issues of child well-being. Two other states—which CDC officials would not name—have had recent preliminary discussions about withdrawing from the state-level data collection, known as the Youth Risk Behavior Survey, said Kathleen Ethier, director of the CDC’s division of adolescent and school health.
“For us, the more data points we have in terms of health and well-being, including mental health, the better positioned we are to try to understand and try to respond to the mental health crisis that we are seeing in this country among young people,” Ethier said. “Data isn’t the only answer, but without the data, we are in the dark.”
April 2022
Blueprint for Youth Suicide Prevention
Even before the COVID-19 pandemic, youth suicides were, sadly, on the rise. Among youth in the United States, more than 25% who die do so from suicide.
During the pandemic, in May 2020, hospital emergency department (ED) visits for suspected suicide attempts began to increase among adolescents aged 12 to 17 years, especially in adolescent girls. From February 21 to March 20, 2021, suspected suicide-attempt ED visits were 50.6% higher among girls aged 12 to 17 years than during the same period in 2019. Among boys in the same age range, suspected suicide-attempt ED visits increased 3.7%.
In 2021 the American Academy of Pediatrics (AAP) and the American Foundation for Suicide Prevention (AFSP), in collaboration with experts from the National Institute of Mental Health (NIMH), created a “Blueprint for Youth Suicide Prevention.” This blueprint is designed to support pediatric health clinicians in advancing equitable youth suicide prevention strategies in all settings in which youth live, learn, work, and spend time.
Psychiatry Advisor, April 29, 2022
Study shows how mental health issues take a toll on college students
To say that college years are a time of great change is an understatement; whether you stay at or close to home, or move away to a four-year university, the post–high school years are often a time of new experiences, unfamiliar responsibilities, growing pains, and learning curves. They can also be a time when some students have to navigate their own physical and mental health for the first time without parental support.
In a new study, Lipson and her colleagues reveal just how common depression, anxiety, and other mental health issues are, and how these issues take a toll on students of color unequally. The paper looks at survey data collected by the Healthy Minds Network between 2013 and 2021 from 350,000 students at over 300 campuses. It’s the first long-term, multicampus study of its kind to parse out differences in treatment and prevalence of mental health issues across race and ethnicity. The study was coauthored by Lipson and other members of the Healthy Minds Network team.
Social Media and Youth Mental Health: How to Find Balance After Pandemic Spikes in Use
Penélope Cruz recently announced on CBS that her children aren’t allowed to use social media until they’re 16.
“I feel really bad for the ones that are teenagers now,” she said. “It’s almost like the world [is] doing some kind of experiment on them: ‘Oh, let’s see what happens if you expose a 12-year-old to that much technology.’”
Cruz may have a point.
According to the American Academy of Child & Adolescent Psychiatry, 90 percent of U.S. teens ages 13–17 use or have used social media.
They’re also using it more frequently.
According to 2020 data from Statista, 63 percent of U.S. parents reported that their teens used more social media than they did before the pandemic.
This rise of social media use in young people coincides with a rise in mental health concerns. Many health experts are calling it a second pandemic.
For instance, according to Mental Health America (MHA), the number of youth who experienced a major depressive episode in 2021 increased by 206,000 from the previous year.
Adolescents accounted for larger share of suicides in many states in 2020
Adolescents accounted for a larger share of suicides across 14 states in 2020 than they did over the previous five years, according to research published Monday.
The findings were described in a research letter in JAMA Pediatrics, as medical groups and health experts increasingly sound the alarm about the soaring mental health challenges of young people.
In October, three prominent children’s health organizations declared that child and adolescent mental health had become a national emergency. The announcement followed a report from the Centers for Disease Control and Prevention, which tracked emergency room visits from suspected suicide attempts before and during the pandemic.
The results showed that in February and March 2021, those visits were 50 percent higher among girls ages 12 to 17 than during the same period in 2019.
College Athlete Suicides Highlight Need for Support, Intervention
As news of another collegiate athlete suicide hits, professionals urge anyone feeling that level of hopelessness to seek professional help immediately.
In March, Stanford University soccer goalie Katie Meyer took her own life and, this weekend, the suicide of University of Wisconsin track star Sarah Shulze was announced. Both women reportedly struggled to balance athletics, academics and daily life.
It’s a familiar struggle for college student athletes, according to Carla Schnitzlein, DO, medical director of Natchaug Hospital, part of the Hartford HealthCare Behavioral Health Network.
“For elite athletes, acknowledging mental health struggles can still be perceived as a weakness,” she explained. “There are a lot of pressures.”
Outcomes generally improve if coaches and other adults support students seeking help, such as in the case of Ohio state football player Harry Miller, who announced his retirement after suicidal intentions, noted Jennifer Ferrand, PsyD, director of well-being for Hartford HealthCare.
Hartford Healthcare, April 25, 2022
Study: Proportion of adolescent suicides rose early in COVID-19 pandemic
Adolescents accounted for a higher proportion of suicides in the United States during the early stages of the COVID-19 pandemic than in the years before the global crisis, a study published Monday found.
In 14 states, the percentage of deaths due to suicide that involved adolescents rose by about 10% in 2020 compared with 2015 through 2019, data published Monday by JAMA Pediatrics showed.
People ages 10 to 19 years in the states included in the analysis accounted for nearly 7% of suicide deaths nationally in 2020, up from an average of just under 6% from 2015 through 2019, the researchers said.
Five of the states included in the analysis–Georgia, Indiana, New Jersey, Oklahoma and Virginia–saw an increase in number of adolescent suicides in 2020 over the previous five-year period, according to the researchers.
‘It’s Life or Death’: The Mental Health Crisis Among U.S. Teens
One evening last April, an anxious and free-spirited 13-year-old girl in suburban Minneapolis sprang furious from a chair in the living room and ran from the house — out a sliding door, across the patio, through the backyard and into the woods.
Moments earlier, the girl’s mother, Linda, had stolen a look at her daughter’s smartphone. The teenager, incensed by the intrusion, had grabbed the phone and fled. (The adolescent is being identified by an initial, M, and the parents by first name only, to protect the family’s privacy.)
Linda was alarmed by photos she had seen on the phone. Some showed blood on M’s ankles from intentional self-harm. Others were close-ups of M’s romantic obsession, the anime character Genocide Jack — a brunette girl with a long red tongue who, in a video series, kills high school classmates with scissors.

In the preceding two years, Linda had watched M spiral downward: severe depression, self-harm, a suicide attempt. Now, she followed M into the woods, frantic. “Please tell me where u r,” she texted. “I’m not mad.”
American adolescence is undergoing a drastic change. Three decades ago, the gravest public health threats to teenagers in the United States came from binge drinking, drunken driving, teenage pregnancy and smoking. These have since fallen sharply, replaced by a new public health concern: soaring rates of mental health disorders.
The New York Times, April 23, 2022
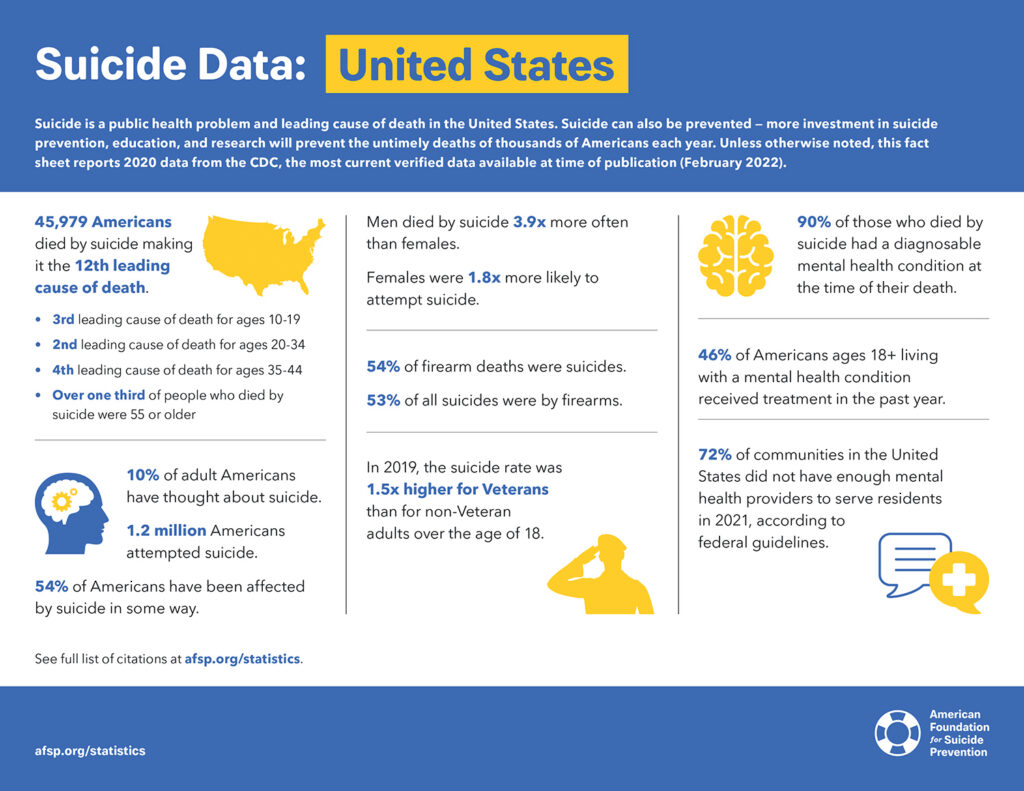

Why American Teens Are So Sad
The Atlantic, April 11, 2022
“The United States is experiencing an extreme teenage mental-health crisis. From 2009to 2021, the share of American high-school students who say they feel “persistent feelings of sadness or hopelessness” rose from 26 percent to 44 percent, according to anew CDC study. This is the highest level of teenage sadness ever recorded.”
“The government survey of almost 8,000 high-school students, which was conducted in the first six months of 2021, found a great deal of variation in mental health among different groups. More than one in four girls reported that they had seriously contemplated attempting suicide during the pandemic, which was twice the rate of boys. Nearly half of LGBTQ teens said they had contemplated suicide during the pandemic, compared with 14 percent of their heterosexual peers. Sadness among white teens seems to be rising faster than among other groups.”
For a PDF of the complete article, go here.
Suicide Rate Decreases by 3 Percent for Second Consecutive Year, According to Most Recent CDC Data (Year 2020)
March 1, 2022
The CDC has released its most recent data related to suicide for the year 2020. Suicide is a leading cause of death, and according to this new data release, the suicide rate went down for the second consecutive year.
In 2020, there were 45,979 suicide deaths; in 2019 there were 47,511 suicide deaths, a decrease of 1,532 deaths. From 2019 to 2020 the over all national U.S. suicide rate declined by 3 percent, including 8 percent among females and 2 percent among males.
Demographic differences in suicide persist, as evidenced by increasing rates among persons aged 25-to-34-years old and 85 and older. Rates increased slightly for Blacks, NativeAmericans/Alaskan Native males and decreased for other age, race and ethnic groups.
For a PDF of the complete article, go here.
Action Alliance Statement on Final CDC Mortality Data Showing Suicide No Longer Top 10 Leading Cause of Death in 2020
The final 2020 mortality data released today by the Centers for Disease Control and Prevention’s (CDC) National Center for Health Statistics show that suicide is no longer a leading cause of death—in large part due to the death toll from COVID-19.
But this in no way means that suicide is not still a critical public health issue, as we can’t assume a downward trend based solely on one or two years of data. In fact, provisional CDC suicide counts for 2020 still show that there were an estimated 45,855 lives lost to suicide in the U.S.—which does not take into consideration the millions of other Americans who experienced suicidal thoughts during this same period.
We also recognize that while it appears age-adjusted suicide rates likely declined in 2020 when compared to 2019, there was also an estimated increase in suicide rates among certain populations, such as Black and American Indian/Alaska Native males. In response, it’s imperative that our country take swift action to make suicide prevention a national priority. Greater, more urgent efforts are needed to 1) strengthen our data collection systems and research investments, 2) ensure equitable delivery of care, and 3) achieve systemic changes, particularly around our crisis response infrastructure.
For a PDF of the complete article, go here.