News Archive: October, November, December 2019
December 2019
Apps don’t provide reliable help for suicide prevention: A study found non-functioning crisis hotline numbers in six apps
A handful of depression management and suicide prevention apps — downloaded millions of times — included incorrect or nonfunctional contact information for suicide crisis help lines, according to a new analysis. While apps can offer people with suicidal thoughts or behaviors an important lifeline, experts are worried that many of the apps available on the Apple App Store or Google Play may not be following best practices, or connecting people with appropriate resources.
Depression management and suicide prevention apps can fill an important role: many people feel more comfortable looking for information or seeking help online, and report that it’s easier to ask questions and share problems online rather than speaking with a person face to face. But that makes it even more important that the digital tools people turn to are up to the highest standards for prevention.
Depression and suicide linked to air pollution in new global study: Cutting toxic air might prevent millions of people getting depression, research suggests
People living with air pollution have higher rates of depression and suicide, a systematic review of global data has found.
Cutting air pollution around the world to the EU’s legal limit could prevent millions of people becoming depressed, the research suggests. This assumes that exposure to toxic air is causing these cases of depression. Scientists believe this is likely but is difficult to prove beyond doubt.
The particle pollution analysed in the study is produced by burning fossil fuels in vehicles, homes and industry. The researchers said the new evidence further strengthened calls to tackle what the World Health Organization calls the “silent public health emergency” of dirty air.
“We’ve shown that air pollution could be causing substantial harm to our mental health, making the case for cleaning up the air we breathe even more urgent,” said Isobel Braithwaite, at University College London (UCL), who led the research.
Few Apps for Depression & Suicide Prevention Meet Clinical Guidelines
Most (93 percent) mobile apps for suicide prevention and depression management do not provide all six suicide prevention strategies commonly recommended in international clinical guidelines, according to a new study led by Nanyang Technological University (NTU), Singapore.
Currently, there are more than 10,000 mental health apps available on the Apple App store and Google Play. But even as digital mental health interventions seem to offer a promising alternative to in-person visits, very few apps available in the app stores have been evaluated in clinical trials or by regulatory bodies.
The study, published online in the journal BMC Medicine, highlights the need for responsible design and creation of guidelines for apps that could have a significant impact on people’s lives.
Suicide Network of Teens Is Linked to 15 Deaths
In November 2019, the British Broadcasting Corporation (BBC) published a documentary on a suicide network of young women on the popular social media application Instagram. Journalist Annemarte Moland works for NRK, a Norwegian government-owned radio and television public broadcasting company. Moland found the online community when she went to a Norwegian town to do a story on 3 teenage girls who had committed suicide. One of the girls had a private Instagram account where she posted thoughts about suicide and self-harm.
This account was part of a network of over 1,000 similar accounts, where young people could share posts on depression, self-harm, and the desire to kill themselves. The average age of girls in this network are 19. There is an unspoken rule throughout these private accounts: don’t snitch. The network offers friendship and support which draws troubled teens to it, but also encourages them to post extreme self-harming images. The darker the post, the more likes and comments it receives. BBC reporter Catrin Nye spoke to one of the girls in the network, “she feels although the Instagram community could be very supportive, she also experienced people saying things like ‘your cut isn’t big enough.’ She says there was a sense of competition as to who was the sickest,” said Nye.
Addiction Center, Dec. 19, 2020
Suicide 30 to 50 Times Higher After ED Visit for Self-Harm, Suicidal Ideation
Findings seen among patients presenting with self-harm and suicidal ideation in California.
Emergency department patients presenting with deliberate self-harm or suicidal ideation are at substantially increased risk for suicide in the year following discharge, according to a study published online Dec. 13 in JAMA Network Open.
Sidra Goldman-Mellor, Ph.D., from the University of California in Merced, and colleagues examined the one-year incidence of suicide and other mortality among emergency department patients (2009 through 2011) who presented with nonfatal deliberate self-harm, suicidal ideation, or any other chief concern. Sociodemographic and clinical factors associated with suicide mortality risk were examined.
Physician’s Weekly, Dec 17, 2019
Massachusetts Case Probes The Role Schools Play In Teen Suicide Prevention
Christina worried when she found her 16-year-old boyfriend, Jacob Goyette, drunk and crying at school in the spring of 2018.
A sophomore at a suburban Massachusetts high school, Christina already knew too many people who had died by suicide. Her mind immediately went to the worst-case scenario.
So Christina says she left Jacob with a friend and headed to the social worker for help. Christina told her she was worried about Jacob’s mental health and says she was promised that word would get to his family.
But Christina says that’s not what happened. Less than two months later, she received the worst news possible: Jacob killed himself in his backyard treehouse.
“They didn’t do anything,” said Christina, who is using her middle name by request of her family to protect her privacy.
Now Jacob’s mother, Shannon Goyette, says she’s planning to sue the school district for failing to protect her son from harm. Goyette’s attorney, Jeffrey Beeler, sent a letter to the school district in September saying it is “inexcusable” that school officials didn’t notify her about Christina’s concerns.
FCC unanimously approves proposal for new 3-digit number as Suicide Prevention Hotline
The Federal Communications Commission is moving ahead with plans to designate a three-digit number to reach the National Suicide Prevention Hotline: 988.
The five-member commission unanimously voted on Thursday to approve the proposal, which is now open for public comment, and start the rulemaking process.
“988 has an echo of the 911 number we all know as an emergency number. And we believe that this three-digit number dedicated for this purpose will help ease access to crisis services, it will reduce the stigma surrounding suicide and mental health conditions, and ultimately it will save lives,” Chairman Ajit Pai said Thursday during the commission’s open December meeting.
The proposal requires carriers to implement 988 as a national suicide prevention hotline within an 18-month timeframe. The FCC is asking for input on “all aspects of implementation,” including whether less or more time is needed.
Using Artificial Intelligence to Strengthen Suicide Prevention
An artificial intelligence tool can identify individuals capable of being trained to help mitigate the risk of suicide.
A team from the University of Southern California (USC) has designed an artificial intelligence algorithm capable of identifying individuals in real-life social groups who could be trained to recognize the warning signs of suicide.
Researchers noted that according to the CDC, the suicide rate for people between the ages of 10 and 24 increased by 56 percent between 2007 and 2017. In comparison to the general population, more than half of individuals who experience homelessness have had thoughts of suicide or have attempted suicide.
The group aimed to examine the potential for social connections such as friends, relatives, and acquaintances to help mitigate the risk of suicide.
Health IT Analytics, Dec.12, 2019
How to See Suicidal Signs Before It’s Too Late
Suicide is the second leading cause of death for people between the ages of 10 and 34. That’s according to the American Psychological Association, which says suicide has increased by 33 percent between 1999 and 2017.
So what are the signs that someone you love, like your child, might be thinking about suicide?
“Change,” said Contact Community Services Crisis Intervention Services Director Cheryl Giarrusso. “Please notice change, because that’s a real indicator that there is something going on. And it could be very subtle change, but if you know your child, or your loved one, or your friend and family member, and you notice a change, ask ‘what’s going on? You seem different and I’m wondering if there is something you’re worried about, concerned about, need to talk about.’ “
It’s hard to identify what’s caused a spike in suicide rates; the APA identifies several contributing factors to suicide like depression, serious mental illness, conditions including pain, stressful life events, or a history of previous attempts or abuse. But Contact Community Services officials say simply asking and being persistent if someone doesn’t speak right away can make a difference.
Hidden Risk Factors in Youth Suicide
Research targets risk factors and interventions for kids at risk for suicide–Anxiety, Poor Sleep, Violence.
With rates of suicide attempts and suicide completions drastically rising for children and adolescents, we need to better understand and recognize hidden risk factors that increase suicidal thoughts and behaviors in youth and to develop new interventions.
The Center for Disease Control and Prevention (CDC) reports that suicide is now the second leading cause of death for those between ages 10 to 17. Ten years ago, suicide was the fourth leading cause of death for this age group.
Psychology Today, Dec. 3, 2019
Concussion May Up Risk for Suicide in High School Students
High school students with a history of sports-related concussions might be at an increased risk for suicide, according to a study published online Nov. 11 in the Journal of Affective Disorders.
Dale S. Mantey, Ph.D., from the University of Texas School of Public Health in Austin, and colleagues used data from the 2017 Youth Risk Behavior Surveillance Survey (13,353 participants) to assess the relationship between self-reported history of sports-related concussion and five risk factors for suicide completion.
The researchers found that overall, 15.0 percent of high school students reported a sports-related concussion in the previous 12 months. Of students who reported a history of concussion, approximately 36 percent reported they had felt sad or hopeless (compared with 31.1 percent of all adolescents) and about 21 percent reported they had thoughts of suicide (compared with 17 percent of all adolescents).
The investigators observed a significant association between self-reported sports-related concussion and greater odds of feeling sad/hopeless (adjusted odds ratio, 1.20), suicidal ideation (adjusted odds ratio, 1.25), suicide attempt (adjusted odds ratio, 1.60), and suicide attempt treated by a doctor/nurse (adjusted odds ratio, 2.35).
Yale Review: How Brain Alterations Contribute to Suicidal Thoughts and Behaviors
How brain alterations contribute to suicidal thoughts and behaviors is the subject of a new published review of brain scanning studies by Yale and international researchers.
Published in Molecular Psychiatry, the review spanned more than two decades of neuroimaging studies and summarized progress made in understanding how alterations in the brain contribute to suicide, now the 10th leading cause of death worldwide.
“The review shows the important advancements that have been made in elucidating the brain circuitry that contributes to suicide risk so the field can provide more targeted and effective suicide prevention strategies,” said Hilary Blumberg, MD, John and Hope Furth Professor of Psychiatric Neuroscience, and Professor of Psychiatry, in the Child Study Center and of Radiology and Biomedical Imaging at Yale. “But there is a great deal more research to do.”
Yale School of Medicine, Dec, 2, 2019
The Crisis in Youth Suicide
Too often, suicide attempts and deaths by suicide, especially among the young, become family secrets that are not investigated and dealt with in ways that might protect others from a similar fate.
The death of a child is most parents’ worst nightmare, one made even worse when it is self-inflicted. This very tragedy has become increasingly common among young people in recent years. And adults — parents, teachers, clinicians and politicians — should be asking why and what they can do to prevent it.
In October, the Centers for Disease Control and Prevention reported that after a stable period from 2000 to 2007, the rate of suicide among those aged 10 to 24 increased dramatically — by 56 percent — between 2007 and 2017, making suicide the second leading cause of death in this age group, following accidents like car crashes.
“We’re in the middle of a full-blown mental health crisis for adolescents and young adults,” said Jean M. Twenge, research psychologist at San Diego State University and author of the book “iGen,” about mental health trends among those born since 1995. “The evidence is strong and consistent both for symptoms and behavior.”
The New York Times, Dec. 2, 2019
Teens and antidepressants: What parents need to know about suicide warnings
Oakwood father questions the role of antidepressants in his son’s suicide death.
An Oakwood father whose teen son died by suicide wants parents to research and ask questions about antidepressants prescribed to their children.
Those drugs come with a warning: “May cause increased thoughts of suicide in children, teens and young adults.”
The so-called “black box” warning is the most serious the Food and Drug Administration can assign to a drug. But it has caused controversy.
Some parents believe they’ve been under-informed about the risks. Doctors, though, fear over-emphasis of the warning scares off patients whose lives could be saved and improved by these drugs.
The Dayton Daily News’ Path Forward project digs into the most pressing issues facing the Miami Valley, including rising concerns about youth mental health. Teen suicide rates in Ohio are at the highest they’ve been since at least 2000.
Dayton Daily News, December 1, 2019
November 2019
Suicide prevention using self-guided digital interventions: a systematic review and meta-analysis of randomised controlled trials
Digital interventions that deliver psychological self-help provide the opportunity to reach individuals at risk of suicide who do not access traditional health services. Our primary objective was to test whether direct (targeting suicidality) and indirect (targeting depression) digital interventions are effective in reducing suicidal ideation and behaviours, and our secondary analyses assessed whether direct interventions were more effective than indirect interventions.
The Lancet Digital Health, Nov. 28, 2019
Poverty. Abuse. Bullying. Many kids are dealing with trauma, and suicide is on the rise
As school leaders, we are responsible for tens of thousands of children. While we can’t see each one of those students every day, we do see many of them — listening in the classroom, studying in the library, laughing in the cafeteria. Whether those students live in Jefferson or Trimble or Harlan or Clay counties, they share similar experiences.
We know that, regardless of where they live, many students come to school with baggage they shouldn’t have to bear: poverty, abuse, parental incarceration, the impact of substance abuse or bullying. As often as we see students who are excited to learn, giggling with their friends, getting help with homework, we understand that there’s so much more to these children that we aren’t seeing.
This year’s KIDS COUNT “County Data Book,” recently released by Kentucky Youth Advocates, is a reminder of the often invisible struggles that many of our students face each day. The book includes a range of data about students’ mental health and the factors that influence it, including suicide.
The data is heart-breaking. Twenty percent of sophomores have harmed themselves on purpose. Eight percent actually attempted suicide. Of children ages 11-14 who died by suicide, 44% experienced problems at school, such as poor grades or incidences of bullying or social exclusion. These data tell us two things: The students in our hallways are grappling with challenges we cannot see, and — far beyond the classroom— we as educators have a moral obligation to address those challenges.
Courier Journal, November 26, 2019
With kids coming home for Thanksgiving, parents need to know the danger signs for suicide risk
While it’s a myth that the suicide rate goes up during the holiday season, suicide among young people is up over the past decade or so, and the Thanksgiving holiday is the first time many parents have seen their kids since dropping them off at college months ago.
According to a local psychotherapist, that makes it a good time for parents to watch for the warning signs for suicide risk.
William McVey, a psychotherapist at the Capital Center for Psychotherapy and Wellness, in D.C., said it’s important to be aware of how your child is talking and acting as they return for the holiday.
It’s important to see whether “they are expressing feelings of hopelessness, if they are talking about everything just being too much of a burden. Many times they’ll express feeling trapped.”
WTPO, Washington, DC, Nov. 27, 2019
Concussions in high school athletes may be a risk factor for suicide
Concussion, the most common form of traumatic brain injury, has been linked to an increased risk of depression and suicide in adults. Now new research suggests high school students with a history of sports-related concussions might be at an increased risk for suicide completion.
The research, which recently appeared in the November issue of the Journal of Affective Disorders, examined the link between self-reported history of concussion and risk factors for suicide completion. It was the first study to include a nationally representative sample of high school students. According to the Centers for Disease Control and Prevention, suicide is the second-leading cause of death in Americans ages 10 to 34.
“It’s important to remember that when it comes to concussions, there’s no visual test to confirm them. Unfortunately, you can’t take your child to have a lab test done to diagnose one,” said Dale Mantey, the study’s lead author, a doctoral student at UTHealth School of Public Health in Austin.
A Snapchat video of a 13-year-old boy’s suicide roiled a Colorado town — and left police chasing social media ghosts
Multiple middle-schoolers in the small community of Dacono reported watching a video of Von Mercado’s death — that then vanished from their phones — frustrating officials and leading to a new state law.
On a May night just after the end of the school year, 13-year-old Von Mercado opened a Snapchat video call and set his cellphone on the ground in his backyard. Then he climbed a ladder next to a tree and stepped off.
The girl he had a crush on, the one who had stopped by earlier that day so he could give her a necklace, ring and fidget spinner, watched on her screen as Von hanged himself, she later told police.
About an hour after his death, police found the black phone on the ground and collected it as evidence, along with Von’s blue Nikes and jean shorts. His phone revealed the boy’s final messages to friends about his plan to “end it all.”
The Colorado Sun, Nov. 25, 2019
How removing ‘likes’ from Instagram could affect our mental health
Today, 500 million people will check their Instagram. And many will keep checking, and checking and checking because humans seem to crave the platform’s visual and social rewards.
But excessive social media use can be problematic, leading to sleep disruption, productivity loss and interpersonal conflicts. While “social media addiction” remains a highly contested term in the scientific community, the similarities between online interactions and addictive behaviors are raising concerns.
That’s why Instagram, which is owned by Facebook, has started testing out a new policy to remove visible likes from the platform. While users could previously see how many likes others had received on their posts, now they will only see the likes on their own photos.
The FCC Chairman Wants to Make It Easier to Call the Suicide Hotline
Under a new plan, people experiencing a mental health crisis could call an equivalent of 911.
There was a period in my life when I carried a small slip of paper in a pillbox in my bag. The paper bore 11 numbers, 1-800-273-8255, that would connect me with the National Suicide Prevention Lifeline. I hoped I’d never need them, and luckily I never did. But having them there, alongside a few ibuprofens and whatever medication I was taking, felt like a literal lifeline during a difficult time. If I needed them, they would be there.
Thanks to the Federal Communications Commission, others struggling with depression and suicidal thoughts might not need that scrap of paper. Calling the suicide hotline could become as easy as dialing 988.
FCC Chairman Ajit Pai announced the proposal Tuesday, setting in motion a process that could formally designate the easy-to-remember three digits as the nationwide suicide hotline. The commission will vote on the plan in December and, if it passes, put it up for public comment.
Orgs release college resource for student suicide “postvention”
AVMA, AAVMC, and AFSP have joined forces on a toolkit to support colleges in the aftermath of student suicide
As part of an ongoing effort to break the stigma surrounding mental health in the veterinary world, three national organizations have partnered on a resource colleges can use in the aftermath of student suicide.
Developed by the American Veterinary Medical Association (AVMA), the Association of American Veterinary Medical Colleges (AAVMC), and the American Foundation for Suicide Prevention (AFSP), After a Suicide: A Toolkit for Colleges of Veterinary Medicine outlines support systems that should be made available for veterinary students, faculty, and staff following the death of a colleague by suicide.
“The tragedy of suicide echoes throughout an organization,” says AAVMC’s chief executive officer, Andrew T. Maccabe, DVM, MPH, JD. “This toolkit provides a best-practices approach to effectively managing the impact of suicide on our academic communities. We’re grateful to the experts in the AFSP, AVMA, and other leaders in our profession who have helped create this important toolkit, and we hope all of our colleges and schools will take full advantage of this excellent resource.”
The free toolkit includes:
• Best practices for how school administrators and staff should respond in the immediate aftermath of a suicide;
• Guidance on helping students, faculty, and staff cope in the short- and long-term;
• Tips on working with the media and community partners (e.g. coroner’s office, local police departments, funeral directors, faith leaders, mental health professionals, etc.);
• Tools for deciding how to safely memorialize students; and
• Information on how to identify and support members of the community who may be vulnerable and reduce the risk of suicide contagion.
Veterinary Practice News, Nov. 21, 2019
9 Things All Parents Should Know About Teens and Suicide
As someone who struggled with suicidal ideation as a teen, I remember how it felt like a dirty little secret—and how little support I had. I can’t imagine how different my experience would have been if I’d had a safe and nonjudgmental environment where I could discuss it out in the open, especially with adults. With teen suicide rates rising, it’s more important than ever that parents know the facts, are familiar with the warning signs, and are equipped with the tools not only to intervene when necessary but to have ongoing conversations with their kids about mental health.
According to an October 2019 Centers for Disease Control and Prevention (CDC) report, the suicide rate in kids, teens, and young adults increased by 56 percent from 2007 to 2017. People between the ages of 10 and 24 are dying by suicide at a rate of 10.6 deaths per 100,000 individuals, up from 6.8 deaths per 100,000 people in 2007. Things become even more upsetting when you focus on certain age ranges, like kids between the ages of 15 to 19, who experienced a 76 percent increase in suicide between 2007 and 2017. In 2017 suicide was the second leading cause of death for people in this age range.
More Adolescents Seek Medical Care For Mental Health Issues
Less than a decade ago, the emergency department at Rady Children’s Hospital in San Diego would see maybe one or two young psychiatric patients per day, said Dr. Benjamin Maxwell, the hospital’s interim director of child and adolescent psychiatry.
Now, it’s not unusual for the emergency room to see 10 psychiatric patients in a day, and sometimes even 20, said Maxwell. “What a lot of times is happening now is kids aren’t getting the care they need, until it gets to the point where it is dangerous,” he said.
ERs throughout California are reporting a sharp increase in adolescents and young adults seeking care for a mental health crisis. In 2018, California ERs treated 84,584 young patients ages 13 to 21 who had a primary diagnosis involving mental health. That is up from 59,705 in 2012, a 42% increase, according to data provided by the Office of Statewide Health Planning and Development.
Kaiser Health News, Nov. 12, 2019
After 4 students died by suicide at Prosper High School, here’s how the district responded
Fourteen-year-old Jack Rohwer. Fifteen-year-old Christian Tyler. Seventeen-year-old Chandler Fetterolf. Eighteen-year-old Braden Speed.
All four were students at Prosper High School. All four died by suicide, the first in 2015.
When Braden passed away in October of last year, just days before the annual suicide prevention walk, the school district didn’t just grieve, it got hyper-motivated. Most importantly, it recognized that things would change only if young people led the way.
This year, students are doing just that in this Collin County community, where the neighborly small-town vibe is fading in a culture of high-achieving, affluent adults with big expectations for their children.
Members of what is known as the Hope Squad are talking candidly about mental health and suicide, seeking out lonely and troubled students, and making referrals to school counselors. So far, squad members have flagged 25 at-risk teens.
The Dallas Morning News, Nov. 11, 2019
Learn signs of teen suicide
The increasing number of suicides nationally among the young and a rise in numbers of attempted suicides punctuate disturbing trends that society needs to address.
Not enough mental health assessment and treatment, too much bullying, and the ever-present and often troublesome social media are among the factors experts cite that contribute to suicides.
A new report from the Centers for Disease Control and Prevention shows the rate of suicides among people ages 10 to 24 rose from 2007 to 2017. In 2007, 6.8 deaths per 100,000 people were reported in that age range, but it jumped to 10.6 deaths per 100,000 in 2017.
And the amount of suicides rose faster from 2013 to 2017 — an average increase of 7 percent per year — compared with 3 percent from 2007 to 2013.
We All Need to Be Educated about Suicide Prevention
Rates are increasing, especially among children and teens. As parents and loved ones are preparing to send their children back to school or off to college, perhaps we need to take time to bring a difficult topic out of the darkness and into the light. Akin to the silent killer hypertension, today we have an emerging silent killer characterized by undetected or unrecognizable emotional distress, that when left untreated may lead to life’s most irreversible outcome: death.
While there has been an increase in suicide rates in the United States, the rates among children and teens presents an even more disturbing picture. Suicide among girls has outpaced suicide among boys. Since 2007, the rates for girls age 10–17 rose by nearly 13 percent compared to 7 percent for boys of comparable age. The rates among adolescents and young adults have reached an all-time high. In fact, suicide among those age 15–19 and 20–24 rose 47 percent and 36 percent respectively since 2000. Suicide has become the second leading cause of death for those age 15–24.
Scientific American, Nov. 6, 2019
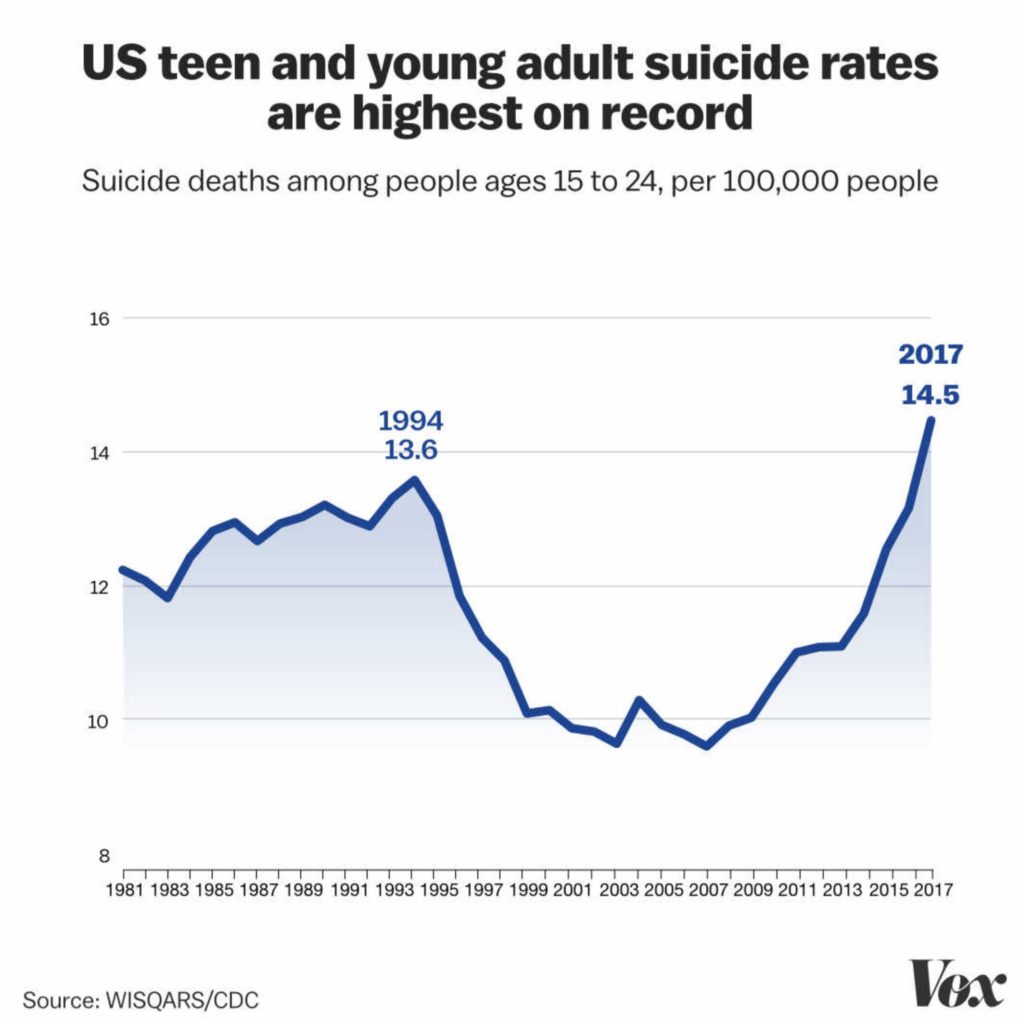
I treat teens who attempted suicide. Here’s what they told me.
Suicide deaths have been rising in recent years. Thoughtful treatment is necessary.
I’ll never forget the first time I cared for a teenager who had made a suicide attempt.
The young man, whom I’ll call Zach, was home from college for winter break. I was a senior medical student completing my clinical rotation in psychiatry. He told me he was having difficulty adjusting to college: He and his roommate weren’t getting along; he missed his brother and parents; and he was beginning to lose touch with friends from high school. Being home, Zach had neither the structure of college, nor the familiar routines he had in high school. I met him after he sustained a serious physical injury when he attempted to end his life.
I wish Zach’s story was a rare occurrence in my career. Unfortunately, over my years in practice, I have been increasingly called on to care for teenagers at risk of suicide, and the stories have only multiplied.
Suicide is the second-leading cause of death (after motor vehicle crashes) in adolescents and young adults, according to Centers for Disease Control and Prevention data, and suicide deaths have been rising for nearly two decades, with an especially concerning spike since 2010. Children’s hospital visits for suicidal thoughts and suicide attempts have doubled since 2008.
Why mental health care deserts persist for U.S. children
Despite an uptick in the number of child psychiatrists nationwide, one out of five U.S. children live in a county with no such provider, according to a study published this week in the journal Pediatrics, which also found that those specialists are largely concentrated in certain pockets of the country. Meanwhile, for various reasons, only half of U.S. children with a mental health condition are receiving treatment.
Nationwide, 70 percent of counties had no child psychiatrists, and children were less likely to have access to professional mental health services if they lived in counties with lower income and education levels. Six states — Idaho, Indiana, Kansas, South Carolina, South Dakota and North Dakota — reported a decline in the number of child psychiatrists during the decade studied.
Risk for Death, Suicide Up in Teens Who Visit ED for Self-Harm
Adolescents with emergency department visits for self-harm have increased rates of recurrent self-harm, mortality, and suicide, according to a study published online Nov. 4 in CMAJ, the journal of the Canadian Medical Association.
William Gardner, Ph.D., from the University of Ottawa in Ontario, Canada, and colleagues used administrative data for 403,805 adolescents aged 13 to 17 years presenting to Ontario emergency departments in 2011 to 2013. A total of 5,661 adolescents with self-harm visits were propensity-matched to 10,731 adolescents who presented for reasons other than self-harm.
Physician’s Weekly, Nov. 4, 2019
Black Teen Suicide Rate Reaches Historic High
African American teenagers in the United States historically have had lower suicide rates than their white counterparts – until now.
“Parents should take heed when they observe specific warning signs like changes in behavior, including difficulty concentrating, difficulty focusing on school or following routine activities, researching ways to kill oneself on the internet, increasing the use of alcohol or other drugs, and acting recklessly,” said Dr. Fran Walfish, a Beverly Hills family and relationship psychotherapist and the author of “The Self-Aware Parent.”
A new study analyzing suicide among American teens by a team led by researchers at the McSilver Institute for Poverty Policy and Research at New York University have uncovered several troubling trends from 1991 to 2017, among Black high school students in particular.
Researchers discovered that between 1991 and 2017, there has been an increase in the number of African American teens who said they had attempted suicide in the past year. Suicide rates for teenagers of other races and ethnicities either remained the same or decreased over that period. The researchers did not cite a reason for the trend.
The Sacramento Observer, Nov. 5, 2019
New Initiative Aims to Prevent Youth Suicide
A teenage boy arrives at Seattle Children’s Emergency Department (ED) with an increased heart rate. His parents are scared and unsure of what could be causing their son’s pulse to spike. While the nurse takes the patient’s vitals, she asks him a series of questions about suicide — prompting the patient to share that he tried to overdose on prescription medication the night before. The nurse informs the provider, and an immediate plan is set in motion to further assess not only the patient’s physical health, but his mental health, as well.
A 10-year-old girl enters the ED with a sprained elbow after taking a tumble on the soccer field. Her parents have been taking her to therapy to help with her anxiety, and the therapist communicates his findings with them often. Because she is so young, the therapist has never directly asked the patient if she’s ever had suicidal thoughts. After the ED nurse initiates suicide-screening questions, the girl admits that she has had thoughts about harming herself in the past.
Seattle Children’s Hospital, Nov. 5, 2019
Media Reports on Celeb Suicides Could Trigger Copycats: How the media reports on celebrity suicides may increase the risk for copycats, a new study suggests.
But following guidelines on the reporting of these suicides can reduce the risk of others following suit, researchers added.
“Suicide needs to be reported on as a public health issue every single time, rather than a story focused on the celebrity’s death and the method of that death,” said researcher Arielle Sheftall, from the Center for Suicide Prevention and Research at Nationwide Children’s Hospital in Columbus, Ohio.
For the study, she and her team used 14 variables from recommendations by the American Foundation for Suicide Prevention on how to report on suicide, which include not sensationalizing the death and framing the report as a public health issue. The researchers looked at how the guidelines were used after the suicides of designer Kate Spade and chef Anthony Bourdain.
After reviewing newspaper articles from across the United States, they found that some media didn’t adhere to several of the suicide reporting guidelines.
On average, only seven of the 14 guidelines were followed and only two were followed by all the newspapers.
U.S. News & World Report, Nov. 1, 2019
Easy access to guns is driving America’s suicide epidemic By Rep. Carolyn Maloney (D-N.Y.)
Our country is experiencing a suicide epidemic. More than 47,000 Americans died by suicide in 2017—an average of 129 per day. It is the 10th leading cause of death in the United States, responsible for more fatalities than many common diseases such as Parkinson’s, liver disease and hypertension. And the problem is getting worse—the suicide rate rose by about 30 percent in the last two decades, with increases for almost every age group.
Easy access to guns is a major cause of these horrifying numbers, according to a new report from my staff on the U.S. Congress Joint Economic Committee. Firearms were used in more than half of suicides in 2017. Approximately 85 percent of suicide attempts with a gun end in death, compared to less than 5 percent without a gun.
There is a clear positive association between levels of household gun ownership and suicide rates. This is true not only for the population as a whole, but also for every age group and both men and women. Access to a firearm triples the risk of death by suicide.
October 2019
One person dies every 12 minutes by suicide; Learn to recognize symptoms and how to help
Nearly 45,000 Americans die by suicide each year — one person every 12 minutes. And for every death there are more than 22 suicide attempts.
To compound the tragedy, suicide can be prevented. It is up to everyone to learn the warning signs and reach out and help those with suicidal thoughts and feelings.
The National Action Alliance for Suicide Prevention and its many national and local community resource partner organizations suggest taking these five steps when you are concerned about someone: Ask, Keep them Safe, Be There, Help them Connect and Follow up.
GoSanAngelo, USA Today, Oct. 28, 2019
Instagram expands ban on suicide content to cover cartoons and memes
Instagram has expanded a ban on graphical self-harm imagery to include a broader range of content depicting suicide, including fictional illustrations of self-harm and suicide methods such as drawings, cartoons and memes.
“This past month, we further expanded our policies to prohibit more types of self-harm and suicide content. We will no longer allow fictional depictions of self-harm or suicide on Instagram, such as drawings or memes or content from films or comics that use graphic imagery,” writes Instagram boss, Adam Mosseri, explaining the latest policy shift. “We will also remove other imagery that may not show self-harm or suicide, but does include associated materials or methods.”
Classmates say 4th grader who died by suicide was bullied
Neighbors are demanding change after a fourth grade boy they say was bullied at school killed himself earlier this week.
Britney Blackwell said the student, who we are not naming out of respect for his family’s privacy, was like family.
“It just broke my heart because now I know that he is not going to come to my house again,” Blackwell told WDEF-TV. “He is not going to give me a hug and say, ‘Hey sister, hey family. I miss you.’ I am not going to see (him) again.”
ABC 13 Eyewitness News, Oct. 27, 2019
Suicide Is Preventable. Hospitals and Doctors Are Finally Catching Up
The suicidal thoughts started when Kristina Mossgraber was 17. A loud voice in her head told her that she was a bad person, a failure, better off dead. She cut herself in secret and told no one about the thoughts slamming around her brain, except her pediatrician, who dismissed them as normal teen angst. But her suicidal thoughts and behaviors didn’t stop. “I was so good at hiding it and kind of normalizing it.” She remembers thinking, “I just need to keep these to myself.”
She did, all through her 20s and early 30s, until one September day in 2014 she drove three hours from her home in Rochester, N.Y., where no one would find her, and cut her neck and the veins down her arms. After struggling to hide her wounds for four days, she went to an emergency room. A doctor sent her home. “They didn’t think I was suicidal enough,” she says.
Most Americans think there is stigma associated with mental illness – CBS News Poll
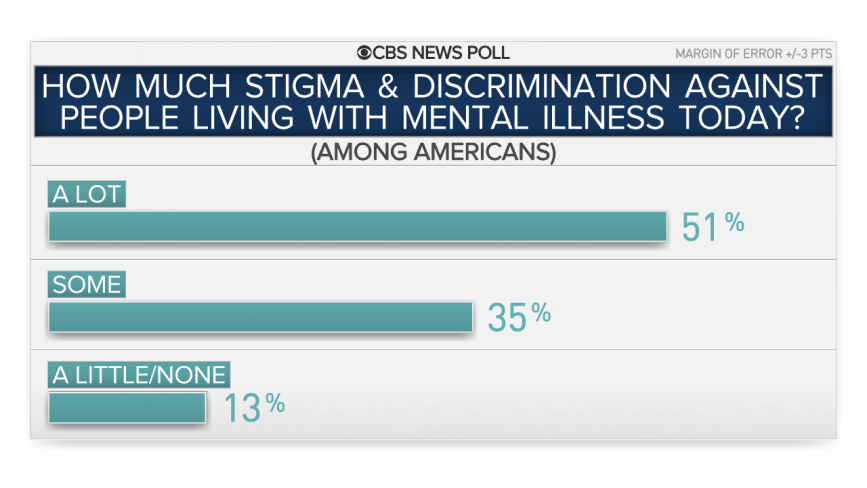
Two in three Americans think mental illness is a very serious public health problem, and few say there are adequate services and support in the U.S. for people living with it. Nearly nine in 10 do think there is at least some stigma and discrimination associated with mental illness in society today, but more than a third say there is less compared to 10 years ago. And this health issue is personal for most Americans: a majority say they personally know someone who has been diagnosed with a mental health disorder.
CBS This Morning, Oct. 23, 2019
Gun Suicide Deaths are Increasing, Costing Billions Per Year, Report Shows
Access to firearms triples the risk of death by suicide, which is having a punishing effect on the U.S. economy, a startling new report from the United States Joint Economic Committee showed.
The report documented the alarming extent to which gun violence and suicide overlap to exact an economic and societal toll in the nation. Using data from the Centers for Disease Control and Prevention (CDC), the report also showed that the rate of suicide has steadily risen, increasing by 30 percent over the past two decades, and suicide and self-harm has cost Americans as much as $70 billion each year.
In 2017, more than 47,000 Americans died by suicide and another 1.4 million attempted it. According to the report, firearms are the leading method for suicide: 51 percent of related deaths are carried out with a firearm. And out of all firearm deaths, 60 percent are attributable to suicide.
Youth suicide rates in CT nearly doubled in one year
The suicide rate among young people in Connecticut nearly doubled in a single year, according to a Hearst Connecticut Media analysis.
Nationwide, suicide rates among 10- to 24-year-olds have increased, the Centers for Disease Control said last week. The suicide rates went from 6.8 for every 100,000 people in 2007 to 10.6 per 100,000 in 2017.
In 2017, suicide was the second leading cause of death for U.S. residents between the ages of 10 and 24, according to the CDC.
Youth suicide rates in Connecticut have fluctuated — 5.35 per 100,000 residents in 2000; 3.73 per 100,000 residents in 2003; 5.57 in 2010; and 4.34 in 2016 — though the rate nearly doubled in 2017 from the previous year.
Connecticut Post, Oct. 21, 2019
Utah researchers identify differences in brains of youth with depression, past suicide attempts
University of Utah researchers say they’ve discovered differences in the way brains of young adults and teens who have experienced depression and suicidal behavior work.
The findings could bring hope to those struggling and might eventually lead to new treatments, researchers say.
“There are lots of worried family members, or family members who have already gone through the heartache of losing someone. And there are lots of patients who might have lost hope that there might be good treatments for them,” said Scott Langenecker, professor of psychiatry at U. Health and senior author on the study published last week in Psychological Medicine.
“Every step we take toward defining some of the biological risk factors for depression and for suicide means we’re one step closer to identifying ways to modify those risk factors.”
Teen Suicide Is on the Rise and No One Knows Why: A new CDC report reveals that teenage suicide rates have increased exponentially in the past decade
A new finding from a Centers for Disease Control report has epidemiologists and mental health experts stumped and concerned. According to the report, teenage suicide rates have increased nearly 56% from 2007 to 2017. The rate of 6.8 deaths per 100,000 people between the ages of 10 and 24 has jumped to about 10.8 deaths. What’s worse, mental health experts have little explanation for what’s driving this increase, making it difficult to know what tack to take in terms of providing early intervention
In itself, the fact that suicide rates among teens are rising is somewhat to be expected: suicide rates have risen across the board over the past few years, rising 33% from 1999 to 2017, according to data from the American Psychiatric Association (APA). Yet the rise in teenage suicides specifically has far outpaced that of the increase in suicides in general. It is now the second-leading cause of death for teenagers, right behind accidental deaths.
CDC Finds Rising Suicide Rates For Young People
A new report by the CDC finds that death rates by suicide have increased for 10-to-24 year-olds between 2007 and 2017.
STEVE INSKEEP, HOST: The number of children and young adults dying by suicide continues to rise, and a new report says the trend affects children as young as 10. The Centers for Disease Control and Prevention published that report. Here’s NPR’s Rhitu Chatterjee.
RHITU CHATTERJEE, BYLINE: Sally Curtin is a statistician with the CDC’s National Center for Health Statistics. She and a colleague looked at deaths by suicide for 10- to 24-year-olds in the 21st century and found that the rate had increased since 2007.
SALLY CURTIN: It increased 56% from 2007 to 2017
CHATTERJEE: For the youngest group, the 10- to 14-year-olds, the rate had nearly tripled to about 500 suicide deaths in 2017. What’s troubling, says Curtin, is that the rise in rates for the entire group has been faster in recent years.
CURTIN: Not only is suicide trending upward, but the pace of increase is actually accelerating.
It Can Take Weeks for College Students to Get the Mental Health Help They Ask For. That’s a Seriously Dangerous Delay. And it needs to change.
Between 2010 and 2016, the number of students seeking on-campus counseling shot up by 30 percent—more than five times the growth of overall college enrollment. The result: By 2018, 34 percent of school health centers reported wait times, per the Association for University and College Counseling Center Directors (AUCCCD). For students on those lists, the average wait time was 17 business days. But at some schools, it stretched to 34.7 days. That’s seven weeks, FYI, or half a semester.
“We’re hearing it more and more,” says Alison Malmon, the founder and executive director of Active Minds, a network of student-run groups that promotes mental health awareness. “What used to be a problem of a two-week wait time has now become four to five weeks.”
Cosmo’s own data confirms these stats. Among the college students we talked to who had asked for counseling, 61 percent said it took a week or more to see someone; 21 percent said more than two weeks.
Half of millennials have left jobs for mental health reasons, survey shows
A new survey examines the role of mental health in the workplace, and the results show that millennials and those part of Generation Z have left jobs for mental health reasons.
According to the survey from Mind Share Partners, a nonprofit organization that tackles issues related to mental health in the workplace, one-fifth of respondents voluntarily left jobs, at least in part, for mental health reasons.
The nonprofit says in the report, which was published in the Harvard Business Review, that this is “a significant finding for companies seeking to recruit and retain talent.”
In addition, more than half of millennials and 75 percent of Gen Zers said they had left a job, at least in part, for mental health reasons. Less than 10 percent of baby boomers said they had left a workplace due to mental health reasons.
Rising suicide rates at college campuses prompt concerns over mental health care
Stanford University has agreed to change its involuntary leave of absence policy, mental health staffing and training to better accommodate students facing mental illness crises, including those who have been hospitalized following a suicide attempt. The decision is the result of a settlement agreement with a group of students who filed a class action lawsuit to reform allegedly discriminatory policies affecting student in mental health crises.
This development is timely as it directly addresses concerns over global suicide trends.
Suicide rates continue to increase across all age groups in America, but the rising youth suicide epidemic, which has progressively increased since the 1950s, is particularly concerning among those who study it.
Young people often turn to common medicine-cabinet drugs when attempting suicide, study says
A new study led by researchers at Nationwide Children’s Hospital indicates that people ages 10 to 25 who attempt suicide by poisoning most often turn to whatever is available–from over-the-counter pain relievers and allergy pills to antidepressants and ADHD medications. They want parents to rethink how they store and manage medications.
Young people attempting to kill themselves by poisoning most often turn to drugs that are found in medicine cabinets and easily accessible at any drug store or grocery, according to a new study.
Over-the-counter analgesics such as aspirin, Tylenol and Advil topped the list of all substances used in nearly 1.7 million suicide attempts nationwide by people ages 10 to 25 from 2000 to 2018, according to the study published online Monday in the journal Clinical Toxicology.
Antidepressants followed, with sedatives and hypnotics the third most commonly used substances. Antihistamines, like Benadryl and other allergy drugs, and antipsychotics rounded out the top five.
The Columbus Dispatch, Oct. 7, 2019
Health Check Kids: Suicide prevention efforts making a difference
Suicide prevention efforts are targeting youth and making a difference in Rhode Island.
In Rhode Island, suicide is the number two cause of death in young people–15 to 24–second only to unintentional motor vehicle accidents.
However, the numbers are going down thanks, in part to a partnership between the state’s Department of Health, the RI assistance program, and Lifespan.
The key is recognizing signs and symptoms.
“Suicidal ideation is not the same as suicide attempts. It’s usually a sign that they feel helpless or hopeless,” said Dr. Jennifer Jencks, assistant director of Lifespan Pediatric Behavioral Health Emergency Services.
Brain Stimulation Shows Promise in Treating Severe Depression
Years ago, more than two dozen patients received an electrical implant to counter their depression. They’re still feeling better, a new study finds.
For more than a decade, doctors have been using brain-stimulating implants to treat severe depression in people who do not benefit from medication, talk therapy or electroshock sessions. The treatment is controversial — any psychosurgery is, given its checkered history — and the results have been mixed. Two major trials testing stimulating implant for depression were halted because of disappointing results, and the approach is not approved by federal health regulators.
Now, a team of psychiatric researchers has published the first long-term results, reporting Friday on patients who had stimulating electrodes implanted as long ago as eight years. The individuals have generally fared well, maintaining their initial improvements. The study, appearing in the American Journal of Psychiatry, was small, with just 28 subjects. Even still, experts said the findings were likely to extend interest in a field that has struggled.
“The most impressive thing here is the sustained response,” Dr. Darin Dougherty, director of neurotherapeutics at Massachusetts General Hospital, said. “You do not see that for anything in this severe depression. The fact that they had this many people doing well for that long, that’s a big deal.”
The New York Times, Oct. 4, 2019
Majority Of U.S. Gun Deaths Are Suicides, But A New Poll Suggests Few Americans Know It
Suicide is the leading cause of gun deaths in the United States, but most Americans don’t know that, according to a new national poll from APM Research Lab, Call To Mind and Guns & America — and experts say that misperception may be handcuffing suicide prevention efforts.
The poll, which asked more than 1,000 Americans what they think the leading cause of gun deaths is, found that 33% of respondents chose homicides outside of mass shootings, while 25% thought that mass shootings caused the most gun deaths
Only 23% said suicides are the leading cause of gun deaths. The remaining respondents chose accidental shootings or said they didn’t know.
WAMU 88.5 American University Radio, Oct. 3, 2019